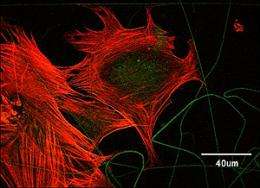
Fluorescence microscopy showing human cells interacting with tropoelastin fibres. Green marks the elastin, red is inside the human cells.
One of the major challenges in stem cell transplants is how to obtain sufficient numbers of these remarkably rare cells to put into patients. To help overcome this issue, research from the Centenary Institute, Royal Prince Alfred Hospital and the University of Sydney has found a way to increase the number of blood-forming stem cells when growing them outside of the body.
By using a unique stretchy surface that allows the cells to pull on it, the researchers found they could generate up to three times more stem cells than using current methods alone. Published today in the leading biotechnology journal Nature Biotechnology, lead author Professor John Rasko from the Centenary Institute and RPA Hospital announced these findings could significantly improve the outcomes of stem cell transplants.
Centenary Institute Head of Gene and Stem Cell Therapy Professor John Rasko said: "Haemopoietic stem cells (HSCs) or blood-forming stem cells play a critical role in creating the blood cells in our body. In order to expand the number of these cells, researchers have attempted to reproduce the unique environment where stem cells live inside the body. In the past we have learnt how to use hormones and drugs to influence these niche environments but less is known about the effect of physical forces.
"Our research has, for the first time, successfully demonstrated that physical forces created by elasticity play a key role in blood-forming cell growth and may mimic the environment of stem cells inside our body. What we've discovered is that blood-forming stem cells like it to be super stretchy because, like a cat on a sofa, they like to pull on their environment."
Dr Jeff Holst#, first author of the publication, combined routinely-used cell hormones with a new elastic-like substance called tropoelastin to coat the plates on which the cells were grown. The study found that growing the stem cells on tropoelastin alone could create as many stem cells as the current hormone-based methods. But the combination of the two produced a super effect with the researchers finding they could create two or three times the number of stem cells than using standard methods on their own.
Professor Tony Weiss^ is a co-author of the Nature Biotechnology paper, and Professor of Biochemistry and Molecular Biotechnology at the University of Sydney. Professor Weiss said: "This is a superb, world class demonstration of leading Australian science. Our inventions are now giving us precise replicas of extraordinarily versatile, natural elastic proteins. By combining our research skills, we have developed a truly impressive technology that we hope will eventually be used to improve the way bone marrow is managed for better medical outcomes."
These findings could be good news for people who receive life-saving stem cell transplants (bone marrow and cord blood transplants) to treat diseased, damaged or faulty stem cells caused by various conditions or treatments such as leukaemia or chemotherapy.
Professor Rasko explained: "By increasing the number of stem cells we can grow outside of the body we could effectively use less bone marrow or cord blood to get the same result or use the same amount to get a much better result. For example, the small quantity of blood used from a cord blood donation often makes it suitable for small children only. Two cord blood donations are usually required to achieve safe transplants in older children or adults. However, in the future, we could use the blood from just one umbilical cord and then increase the number of stem cells to a viable level outside of the body before transplanting these life-saving cells into patients."
Provided by Centenary Institute