In the aftermath of a heart attack, the body's own defenses may contribute to future heart failure. Authors of a new study believe they have identified a protein that plays an important role in a process that replaces dead heart muscle with stiffening scar tissue. The researchers are hopeful that the findings will lead to the development of new therapies to prevent this damage.
"The body tries to fix the injury to the heart muscle by depositing the fibers, but this causes a greater problem," says Dr. Thomas Sato, co-senior author of the study and the Joseph C. Hinsey Professor in Cell and Developmental Biology at Weill Cornell Medical College in New York City. "This process, called fibrosis, causes the heart to become like steel, unable to contract and pump blood throughout the body. The result can be fatal."
Myocardial infarction causes 13 percent of deaths worldwide and is the leading cause of death in industrialized countries.
The researchers' promising findings were published online, Dec. 14, in Nature Cell Biology and will be featured in the upcoming January issue. Due to the findings' significance, the journal has selected the study as an issue highlight.
"Treatments for fibrosis in the heart are relatively limited, making it important to develop new and novel approaches to limit fibrosis," explains Dr. Craig Basson, co-author of the study, the Gladys and Roland Harriman Professor of Medicine and director of the Center for Molecular Cardiology at Weill Cornell Medical College, and attending physician at NewYork-Presbyterian Hospital/Weill Cornell Medical Center.
Dr. Sato and his team removed from a mouse's genome a gene called Sfrp2, stopping the mice from producing the protein sFRP2. They found that there was less scar tissue formed in the hearts of mice without the gene, compared to normal mice that still had the gene within their DNA.
The experimental mice also had improved recovery to their heart function, which leads the authors to believe that the protein has a direct affect on muscle scarring and stiffening following myocardial infarction.
The Weill Cornell team collaborated with Dr. Daniel S. Greenspan, co-senior author and professor of pathology and laboratory medicine from the University of Wisconsin School of Medicine and Public Health in Madison, Wis. Dr. Greenspan determined how the main component of connective tissue, collagen, interacts with the sFRP2 protein, and how these molecules play a crucial role in scar formation.
"With many injuries and diseases, large amounts of collagen are formed and deposited in tissues, leading to scarring and fibrosis," says Dr. Greenspan, an expert in collagen. "Fibrosis can severely affect the functioning of the heart, lung, liver and other tissues."
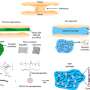
Together, the researchers determined that the sFRP2 protein works by accelerating the processing of pro-collagen, a precursor of mature collagen, the main component deposited in scar tissue. Following a heart attack, fibrous collagen deposits are increased, replacing the dead muscle and leading to more scar tissue, which prevents recovery.
"Therapeutically, the findings mean that it is possible to create a drug that may one day inhibit the functioning of the protein in order to limit fibrosis within the heart," says Dr. Sato. "Doing so may aid in controlling the degree of scarring, and allow the heart to continue to function following myocardial infarction."
Source: New York- Presbyterian Hospital