Study identifies genetic changes likely to have enabled SARS-CoV-2 to jump from bats to humans

A new study, involving the University of Cambridge and led by the Pirbright Institute, has identified key genetic changes in SARS-CoV-2—the virus that causes COVID-19—that may be responsible for the jump from bats to humans, and established which animals have cellular receptors that allow the virus to enter their cells most effectively.
The genetic adaptions identified were similar to those made by SARS-CoV—which caused the 2002-2003 SARS epidemic—when it adapted from bats to infect humans. This suggests that there may be a common mechanism by which this family of viruses mutates in order to jump from animals to humans. This understanding can be used in future research to identify viruses circulating in animals that could adapt to infect humans (known as zoonoses) and which potentially pose a pandemic threat.
"This study used a non-infectious, safe platform to probe how spike protein changes affect virus entry into the cells of different wild, livestock and companion animals, something we will need to continue monitoring closely as additional SARS-CoV-2 variants arise in the coming months," said Dr. Stephen Graham in the University of Cambridge's Department of Pathology, who was involved in the study.
In the 2002-2003 SARS epidemic, scientists were able to identify closely related isolates in both bats and civets—in which the virus is thought to have adapted to infect humans. However, in the current COVID-19 outbreak scientists do not yet know the identity of the intermediate host or have similar samples to analyze. But they do have the sequence of a related bat coronavirus called RaTG13 which shares 96 percent similarity to the SARS-CoV-2 genome. The new study compared the spike proteins of both viruses and identified several important differences.
SARS-CoV-2 and other coronaviruses use their spike proteins to gain entry to cells by binding to their surface receptors, for example ACE2. Like a lock and key, the spike protein must be the right shape to fit the cell's receptors, but each animal's receptors have a slightly different shape, which means the spike protein binds to some better than others.
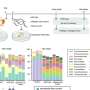
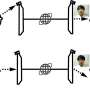
To examine whether these differences between SARS-CoV-2 and RaTG13 were involved in the adaptation of SARS-CoV-2 to humans, scientists swapped these regions and examined how well these resulting spike proteins bound human ACE2 receptors—using a method that does not involve using live virus.
The results, published in the journal PLOS Biology, showed SARS-CoV-2 spikes containing RaTG13 regions were unable to bind to human ACE2 receptors effectively, while the RaTG13 spikes containing SARS-CoV-2 regions could bind more efficiently to human receptors—although not to the same level as the unedited SARS-CoV-2 spike protein. This potentially indicates that similar changes in the SARS-CoV-2 spike protein occurred historically, which may have played a key role in allowing the virus to jump the species barrier.
Researchers also investigated whether the SARS-CoV-2 spike protein could bind to the ACE2 receptors from 22 different animals to ascertain which of these, if any, may be susceptible to infection. They demonstrated that bat and bird receptors made the weakest interactions with SARS-CoV-2. The lack of binding to bat receptors adds weight to the evidence that SARS-CoV-2 likely adapted its spike protein when it jumped from bats into people, possibly via an intermediate host.
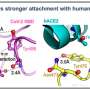
Dog, cat, and cattle ACE2 receptors were identified as the strongest interactors with the SARS-CoV-2 spike protein. Efficient entry into cells could mean that infection may be more easily established in these animals, although receptor binding is only the first step in viral transmission between different animal species.
"As we saw with the outbreaks in Danish mink farms last year, it's essential to understand which animals can be infected by SARS-CoV-2 and how mutations in the viral spike protein change its ability to infect different species," said Graham.
An animal's susceptibility to infection and its subsequent ability to infect others is reliant on a range of factors—including whether SARS-CoV-2 is able to replicate once inside cells, and the animal's ability to fight off the virus. Further studies are needed to understand whether livestock and companion animals could be receptive to COVID-19 infection from humans and act as reservoirs for this disease.
More information: Carina Conceicao et al. The SARS-CoV-2 Spike protein has a broad tropism for mammalian ACE2 proteins, PLOS Biology (2020). DOI: 10.1371/journal.pbio.3001016
Journal information: PLoS Biology
Provided by University of Cambridge