Factor found to balance medically useful stem cell qualities
A key protein controls stem cell properties that could make them more useful in regenerative medicine, according to a study led by Mount Sinai researchers and published online today in the journal Cell Stem Cell.
Each of us develops from an unspecialized single cell into hundreds of different specific cell types. Stem cells multiply (proliferate) and mature (differentiate) in the womb to become muscle, bone, nerves, etc. To make stem cells the basis for safe medical treatments, however, the field would need the ability to tightly control stem cell pluripotency, the ability to become many cell types, and self-renewal or immortality, the ability to keep dividing and multiplying over time in constant turnover.
This elusive stability must be achieved before stem cell supplies can be kept on hand until it is time to turn them into replacements for say misshapen red blood cells seen in sickle cell anemia or abnormal white blood cells causing leukemia. Also limiting the use of therapeutic stem cells to date, self-renewal, a quality so vital to a fast-growing fetus, can also be a source of cancer risk when haphazard, unlimited cell multiplication results in the abnormal tissue growth seen in tumors.
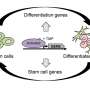
In the current study, Mount Sinai researchers found that the protein called "zinc finger protein 217" (ZFP217) regulates the actions of genes that maintain a balance between stem cell self-renewal and differentiation. The study results were found using mouse embryonic stem cells, which are good cell models for the study of processes seen in human stem cells.
"The hope is that ZPF217 could be used to maintain supplies of therapeutic stem cells," said lead study author Martin Walsh, PhD, Associate Professor of Pediatrics, Structural and Chemical Biology, and Genetics and Genomic Sciences of the Icahn School of Medicine at Mount Sinai. "At the same time, as the human ZNF217 is associated with poor survival in a variety of cancers, understanding how this protein operates in physiological conditions may help to predict cancer risk, achieve earlier diagnosis and provide novel therapeutic approaches."
The study results build on genetic and epigenetic basics, including that the blueprint for the human body is encoded in genes that direct the building of one or more proteins. Gene expression is the process where information stored as DNA is converted (transcribed) by enzymes into related molecules called RNAs, and then into proteins that make up the body's structures and signals.
A transcriptome is the set of all RNA molecules transcribed in each cell type, and a readout on which genes are turned in that cell at the time. DNA is transcribed into messenger RNA (mRNA) that carries the code to ribosomes, the molecular machines that build proteins by reading the mRNA instructions. At several points in the process of turning on genes, transcribing them into RNAs, and then translating them into proteins, chemical changes may occur that either encourage or interfere with that gene expression.
This is the science of epigenetics, in which chemical changes to genetic material turn genes on or off without changing the order of the DNA code inherited from your parents. Methylation, the chemical attachment at a certain point on the DNA chain of a methyl group (one carbon atom bonded to three hydrogen atoms), is a common type of epigenetic, regulatory change that can "silence" a gene.
While many epigenetic mechanisms regulate genetic function at the level of DNA, an emerging science looks at regulation through chemical changes to RNAs in yet another level of regulatory finesse.
N6-Methyladenosine (m6A) is the most commonly occurring RNA modification in human cells, influencing the stability and its ability to carry genetic messages. In the current study, ZFP217 was found to regulate m6A deposition on to mRNAs created by stem cell pluripotency genes by attaching to another enzyme, m6A methyltransferase-like 3 (METTL3), and rendering it inactive. This prevents methylations that would otherwise cause the stem cells to differentiate, putting an end to their self-renewal and pluripotency.
At the same time, the study results provide further argument for notion that m6A methylation, partly controlled by ZFP217 signaling, is relevant in human cancers. Overexpression of ZNF217 provides an advantage to tumor cells by allowing cells to infinitely proliferate and turning down pathways that typically tell cells to mature into functional cells (bone, blood, skin cells).
The research team also found that ZFP217 turns on the genes important for stemness, including Nanog and Sox2. ZFP217 expression may in turn be influenced by these same factors in the kind of feedback loop seen in complex genetic regulation.
Since 2006, researchers have been able of take differentiated specialized cells, like skin cells, and transform them into induced pluripotent stem cells or iPSCs. Such iPSCs are genetically specific to that patient. This offers the promise of creating personalized, therapeutic stem cells. Nanog and Sox2 are among the enzymes used by researchers to generate iPSCs, therefore ZFP217 may represent another tool needed to achieve tight control over cell reprogramming.
Journal information: Cell Stem Cell
Provided by The Mount Sinai Hospital