Neutron studies of HIV inhibitors reveal new areas for improvement in drug design to enhance performance, combat resista
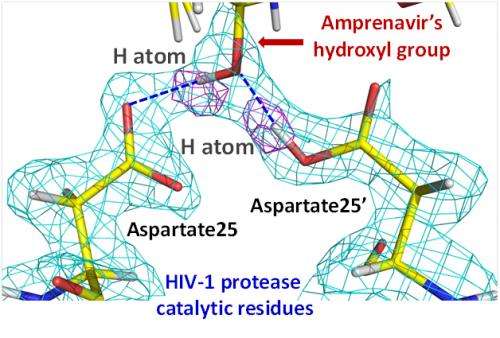
The first study of interactions between a common clinical inhibitor and the HIV-1 protease enzyme has been carried out by an international team with members from the US, Britain and France using neutrons at the Institut Laue-Langevin in Grenoble, France. It provides medical science with the first true picture of how an antiviral drug used to block virus replication actually works, and critically how its performance could be improved.
The findings, reported in the Journal for Medicinal Chemistry, and the neutron techniques demonstrated at the ILL, will provide the basis for the design of a new generation of more effective pharmaceuticals to address issues such as drug resistance.
HIV-1 protease is essential in the life-cycle of HIV where it breaks polypeptide chains to create proteins used for replication and producing new infectious virus particles. Its key role makes it one of the most studied enzymes in the world. For the past 20 years scientists have used highly intense X-rays to investigate the best way to target and block the protease's role in spreading the virus.
However, this form of analysis has limitations. The strongest bonds between the enzyme and an inhibitor are usually relatively weak hydrogen bonds, yet hydrogen atoms are virtually invisible to X-ray analysis, leaving scientists to speculate as to how this binding takes place.
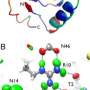
To address this uncertainty, scientists from Georgia State University, Purdue University and Oak Ridge National Laboratory in the USA and Harwell Oxford in Great Britain used neutrons at the Institut Laue-Langevin to analyse this binding. Neutrons are highly sensitive to lighter elements, allowing the team to identify the positions of every hydrogen atom involved in the system for the first time, and see which were involved in bonding. The inhibitor studied was Amprenavir (APV), first approved for clinical use in 1999, and experiments were carried out on the LADI-III (quasi-Laue neutron diffractometer) instrument at the ILL.
The neutron studies revealed a very different picture to that inferred from the X-ray studies which had overplayed the importance of many of the hydrogen bonds. In fact the team found only two really strong hydrogen bonds between the drug and the HIV enzyme.
Whilst this might seem concerning, it actually presents drug designers with a set of new potential sites for the improvement of the drug's surface chemistry to significantly strengthen the binding, thereby increasing the effectiveness of the drugs and reducing the necessary dosages.
Based on their new understanding the team proposed a number of next steps to make these improvements, including:
- Replacing weaker bonds with a greater number of stronger hydrogen bonds - Now it is known that many of the bonds are actually weak and water-mediated, drug designers should look to replace these with stronger hydrogen bonds. This could be done by changing certain functional groups in the drug chemical structure in order to expel water currently filling the holes.
- Improving the strength of the existing hydrogen bonds - For example lowering the pKa (the ability or tendency of a compound to lose its hydrogen atoms) of certain chemical groups of the drug to make it more similar to that of the enzyme would make the hydrogen atoms in the bond equidistant between the two compounds, resulting in a stronger interaction.
The findings in this latest paper may also help address one of the biggest issues in combating HIV infection - drug resistance. The natural evolution of the virus overtime weakens the binding, a process which is actually sped up by the introduction of the drugs themselves. One way round this would be to improve the binding of the inhibitor with the main-chain atoms of the virus's protease (rather than its side chains), which cannot mutate.
Before this latest study it was thought the potential for advances in this area was limited because the hydrogen bond interactions with the main-chain atoms were already considered strong. However, this has been shown not to be the case, creating a new avenue for the development of HIV pharmaceuticals much less affected by virus evolution and resistance.
Dr Matthew Blakeley, Institut Laue-Langevin said: "This study perfectly illustrates the benefits of neutrons in drug design due to their unique sensitivity to hydrogen atoms. Until recently high-resolution neutron studies of large biological systems were restricted due to the size of crystals that needed to be grown and the length of time it took for the results to be collected. However, significant technical developments, led by pioneering work here at the ILL, have greatly extended the range of experiments that can be performed providing the pharma industry with a powerful new tool to improve the performance of their products."
More information: Weber, I. et al. Joint X-ray/Neutron Crystallographic Study of HIV-1 Protease with Clinical Inhibitor Amprenavir: Insights for Drug Design Re.: J. Med. Chem., 2013, 56 (13), pp 5631–5635. DOI: 10.1021/jm400684f
Provided by Institut Laue-Langevin