A collaboration solves the herpes virus protein structure providing new drug therapy directions
The mechanism by which a herpes virus invades cells has remained a mystery to scientists, but now research from Tufts University and the University of Pennsylvania reveals the unusual structure of a key member of the protein complex that allows a herpes virus to invade cells.
The new map details an essential piece of the herpes virus "cell-entry machinery," providing scientists with a new target for antiviral drugs.
The research was published online in the journal Nature Structural & Molecular Biology.
Researchers at Tufts and Penn used X-ray crystallography along with cell microscopy techniques to study the structure and function of the cell-entry protein fusion events carried out by HSV-2. The research has resulted in a map of an important protein complex required to trigger herpes virus infection, setting the stage for new therapeutics that may prevent the virus's access to cells.
Most viruses need cell-entry proteins called fusogens in order to invade cells. Scientists have known that the herpes virus fusogen does not act alone, requiring a complex of two other viral cell-entry proteins. In this study, researchers determined the structure of this key protein complex and realized it did not resemble the structure of other known fusogens.
"This unexpected result leads us to believe that this protein complex is not a fusogen itself but that it regulates the fusogen," said senior author Ekaterina Heldwein, assistant professor of molecular and microbiology at Tufts University School of Medicine. "We also found that certain antibodies interfere with the ability of this protein complex to bind to the fusogen, evidence that antiviral drugs that target this interaction could prevent viral infection."
"We hope that determining the structure of this essential piece of the herpes virus cell-entry machinery will help us answer some of the many questions about how herpes virus initiates infection," said first author Tirumala K. Chowdary, a postdoctoral associate at Tufts. "Knowing the structures of cell-entry proteins will help us find the best strategy for interfering with this pervasive family of viruses."
There is no cure for herpes viruses. Upon infection, the viruses remain in the body for life and can stay inactive for long periods of time. When active, however, different herpes viruses can cause cold sores, blindness, encephalitis or cancers. More than half of Americans are infected with herpes simplex virus type 1, HSV-1, by the time they reach their 20s. About one in six Americans is infected with herpes simplex virus type 2, HSV-2, which is the virus responsible for genital herpes. Complications of HSV-2, a sexually-transmitted disease, include recurrent painful genital sores, psychological distress and, if transmitted from mother to child, potentially fatal infections in newborns.
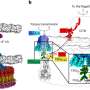
Herpes viruses, which cause many incurable diseases, infect cells by fusing viral and cellular membranes. Whereas most other enveloped viruses use a single viral catalyst called a fusogen, herpes viruses inexplicably require two conserved fusion-machinery components, gB and the heterodimer gH-gL, plus other nonconserved components. gB is a class III viral fusogen, but, unlike other members of its class, it does not function alone.
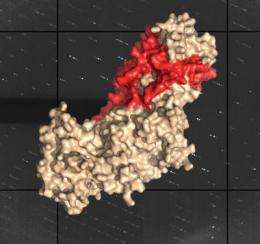
"We determined the crystal structure of the gH ectodomain bound to gL from herpes simplex virus 2," said Roselyn J. Eisenberg, professor of microbiology at the University of Pennsylvania School of Veterinary Medicine. "gH-gL is an unusually tight complex with a unique architecture that, unexpectedly, does not resemble any known viral fusogen."
"We propose that gH-gL activates gB for fusion, possibly through direct binding," said Gary Cohen, professor of microbiology at the University of Pennsylvania School of Dental Medicine. "Formation of a gB-gH-gL complex is critical for fusion and is inhibited by a neutralizing antibody, making the gB-gH-gL interface a promising antiviral target."
Provided by University of Pennsylvania