New antimicrobial surface reduces bacteria build-up on medical instruments

Monash University researchers have engineered new antimicrobial surfaces that can significantly reduce the formation of bacteria on medical instruments, such as urinary catheters, and reduce the risk of patient infection while in hospital.
This world-first study demonstrates the potential for 3D engineered surfaces in preventing the initial formation of microcolonies of Escherichiacoli (E.coli), Klebsiellapneumoniae and Pseudomonas aeruginosa—the three most common urinary tract bacterial infections (UTIs) associated with catheters.
The study team, led by Dr. Victor Cadarso, from Monash University's Department of Mechanical and Aerospace Engineering and the Center to Impact AMR, engineered surfaces with smooth, 3D micro features, instead of the traditional sharp cross-sectional ones, to reduce the potential for harmful bacteria to attach on these surfaces in large numbers.
The tested surfaces demonstrated reduction in both attachment of bacteria and biofilm formation. One of the surfaces, P01, presented excellent properties against E.coli, K.pneumoniae, and P. aeruginosa with 55 percent, 69 percent and 68 percent less bacterial cells attached, and 53 percent, 77 percent and 66 percent less microcolonies being formed, respectively.
Urinary tract infections (UTIs), associated with urinary catheters, are the most common type of healthcare-associated infections. They have been identified by the World Health Organization (WHO) as an urgent global health threat.
Approximately one in five of hospitalized patients globally are administered urinary catheters during their hospital stay. It is estimated that 13,000 people across the world die each year from UTIs, and a further 700,000 die from associated antimicrobial resistance infections because of the resistance of superbugs to antibiotics and current sterilization methods.
The study was published in the international journal ACS Applied Materials & Interfaces. Researchers from Monash University's Department of Microbiology were also involved and part of the work was done at the Melbourne Center for Nanofabrication.
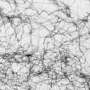
"Using E.coli as an example, we found bacterial cells that form on surfaces do so mostly on the sharp corners. By removing these sharp features, the bacteria can no longer colonize the surface as effectively. This same effect has been demonstrated for the two other pathogens in this study," said Sara Ghavamian, from the Monash Department of Mechanical and Aerospace Engineering, who created these surfaces.
"High-touch surfaces within hospitals, such as catheters and ventilators, are a significant source of microbial spread and healthcare-associated infections.
"Infection control through physically altering the micro architecture of these surfaces, rather than the traditional use of chemical agents, is not only a more durable approach but also an effective strategy for combating antimicrobial resistance."
The bacterial colonization of surfaces takes place over time. Once bacteria attach to a surface, a series of cellular responses are triggered. After this initial phase, including a few rounds of cell division by this bacteria, microcolonies of hundreds of bacterial cells are formed.
After successful colonization, the bacteria form a biofilm—a large population of bacteria in a 'secreted cellular matrix' that binds together and protects the cells from antibiotics and the immune system. This might create a superbug that can cause long-term health implications for patients.
Researchers demonstrated that their 3D engineered microtopographies with varying heights and smooth curved cross-sections can simultaneously deter both the initial attachment and the formation of biofilms for three clinically relevant bacteria.
Through an extensive screening process, researchers identified that the sharp corners of the vertical side walls within the conventional micropatterned surfaces gifted bacteria with perfect hiding spots to shelter themselves against the flow of fluids which could wash them away.
The researchers hypothesize that by smoothing out these corners, the bacteria would be left with nowhere to hide.
"After equivalent incubation periods with the same bacteria, we discovered that while the micropatterned surfaces were indeed successful in reducing the number of microcolonies formed they, problematically, increased the number of attached bacteria compared with traditional micro-flat surfaces," Sara said.
"Opposite the conventional sharp micropatterned surfaces, our smooth design demonstrated a simultaneous decrease in both the number of bacterial attachment and microcolony formation compared to the standard flat surfaces.
"Developing strategies to prevent the bacterial colonization of surfaces, such as catheters, without requiring antimicrobial drugs or chemicals is critical to stop biofilm formation and the potential spread of harmful diseases."
More information: Sara Ghavamian et al, Three-Dimensional Micropatterning Deters Early Bacterial Adherence and Can Eliminate Colonization, ACS Applied Materials & Interfaces (2021). DOI: 10.1021/acsami.1c01902
Journal information: ACS Applied Materials and Interfaces
Provided by Monash University