Scientists uncover how the Wntless protein carries Wnts in its signalling pathways
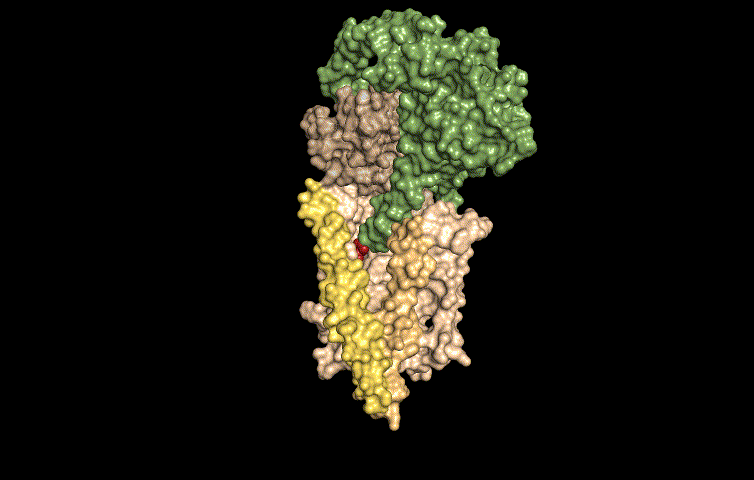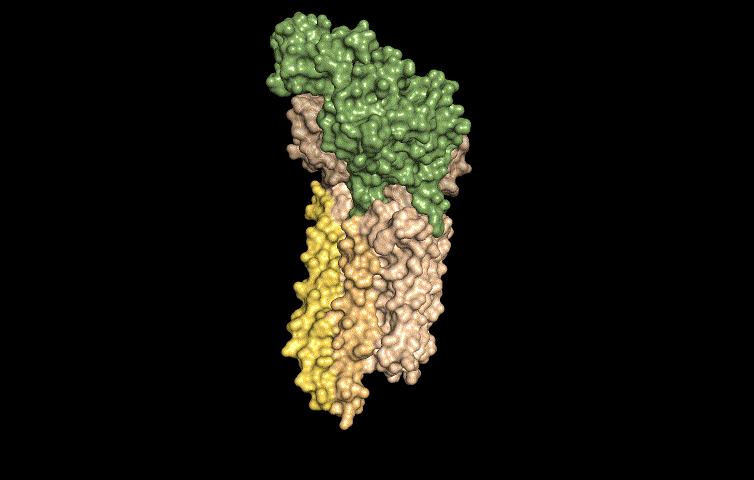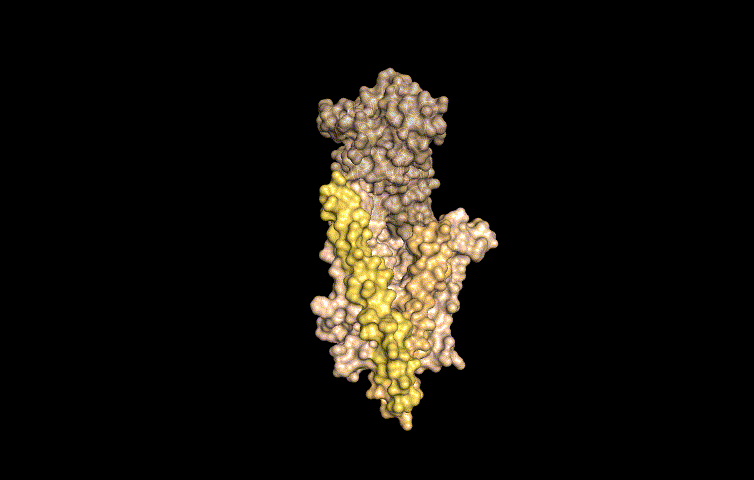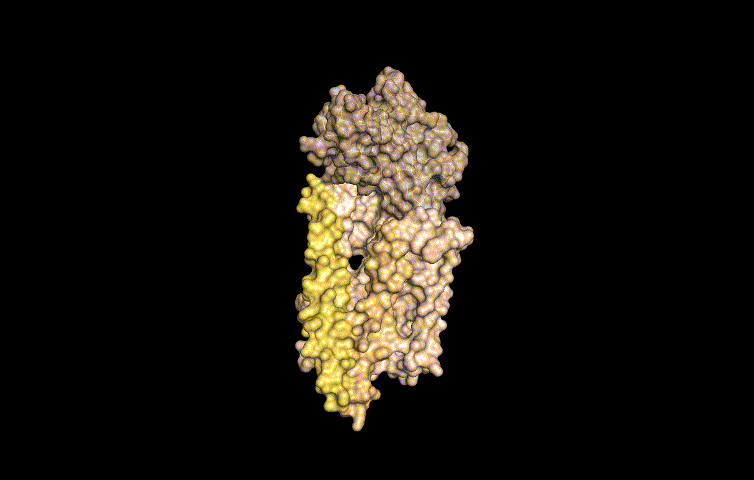
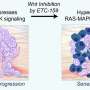
Researchers from Duke-NUS Medical School in Singapore and Columbia University in the U.S. have solved how Wnt proteins, which play a fundamental role in cell proliferation and differentiation, hitch a ride to travel from their cellular factory to the cell surface. Drugs that interfere with Wnt transport, like the made-in-Singapore anti-cancer drug ETC-159, can be used to treat diseases with excess Wnt signaling, such as cancer and fibrosis.
"Since excessive Wnt signaling can drive cancer, supress immunity and trigger fibrosis, there is great interest in trying to block this transport link," said Professor David Virshup, the director of Duke-NUS' Cancer and Stem Cell Biology Programme and a corresponding author of the study.
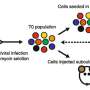
Wnts are proteins that send signals from cells to tell tissues and organs what is going on around them. Animals from sponges and jellyfish to humans rely on Wnt signaling to build their body plans. In adult humans, Wnt continues to control functions, including maintaining hair, intestines and tastebuds. Unlike most other cell-to-cell signaling proteins, however, Wnts have a fatty acid attached to them. Because of this attached fatty acid, Wnts require a dedicated transporter protein, called Wntless (WLS).
But how the WLS protein actually carries the fatty acid-modified Wnt signal around cells and between cells has not been understood.
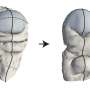
In this work, published last week in Cell, the researchers determined the molecular structure of Wnt as it is being carried by Wntless using cryo-electron microscopy. This method allowed the researchers to study the structures of the two proteins in a near native state without interference from the staining or fixing required by traditional electron microscopy.
"We determined the structure of the short-range signaling molecule Wnt in complex with WLS. The structure explains why these two proteins form such a tight complex, as we observe a very large binding surface between the two proteins," said Filippo Mancia, an associate professor of Physiology and Cellular Biophysics at Columbia University Medical Center and the co-corresponding author of the study.

"The structure also reveals how the fatty acid attached to Wnt can be shielded in the membrane when bound to WLS and helps to explain why a receptor, such as WLS, is necessary to transport Wnt from inside the cells to the cell membrane," added Rie Nygaard, an associate research scientist in the Mancia Lab, who led the structural biology component of the project.
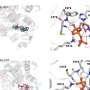
The structure revealed that WLS has two domains: a transmembrane domain and a second domain that resembles an ancient fatty acid regulator. The fatty acid tail of Wnt is inserted into a conserved cavity in the transmembrane domain of WLS.
The transmembrane domain where the fatty acid tail binds is a promising drug target as it is structurally related to the family of G-protein-coupled receptors (GPCRs), which have been found to be very druggable.
"What's even more encouraging for us is that we already have a candidate drug that blocks this particular interaction and that's ETC-159," said Yu Jia, who is one of the authors of the study and a Senior Research Fellow at Duke-NUS' Cancer and Stem Cell Biology Programme.
ETC-159 is a made-in-Singapore anti-cancer drug, which was jointly developed by Duke-NUS and the Experimental Drug Development Centre (EDDC), a national platform for drug discovery and development hosted by A*STAR, the Agency for Science, Technology and Research. The Wnt-inhibitor is a novel small-molecule drug candidate that targets a range of cancers. It is currently progressing through clinical trials as a treatment for a subset of colorectal and gynecological cancers.
Over the next year or so, the researcher team hopes to build on this structure to understand in detail how Wnts get loaded onto WLS and how WLS is delivered to its receptors.
More information: Rie Nygaard et al. Structural Basis of WLS/Evi-Mediated Wnt Transport and Secretion, Cell (2020). DOI: 10.1016/j.cell.2020.11.038
Provided by Duke-NUS Medical School