Proof-of-concept technique makes nanoparticles attractive for new medications
Since the development of insulin to manage diabetes, pharmacists have longed to create an insulin pill. Past attempts have failed because insulin does not survive the harsh conditions of the gastro-intestinal (GI) system and cannot easily cross the GI wall. Researchers at University of Utah Health developed a proof-of-concept technology using nanoparticles that could offer a new approach for oral medications. The results will be published online in the August 8 issue of the journal ACS Nano.
"In the pharmaceutical world, this has been regarded as the holy grail," said You Han Bae, Ph.D., professor Pharmaceutics and Pharmaceutical Chemistry at U of U Health and senior author on the paper.
Nanomedicine is a burgeoning field of medicine that delivers tiny particles (nanoparticles) to carry drugs to treat a variety of conditions, including cancer. These treatments are commonly given intravenously, because solid nanoparticles have a poor absorption rate in the body.
Bae and his team modified the surface of the nanoparticles with glycocholic acid, a bile acid that helps the body absorb fat in the small intestine.
The glycocholic acid acts like a cloak, allowing the nanoparticle to slip incognito through the lining of the small intestine. Preliminary evidence suggests that the coating helps the nanoparticles bind to proteins that let them move into the gut lymphatic system where it can access the bloodstream.
"Nanoparticles were not expected to be absorbed through the lymphatic system," said Kyoung Sub Kim, Ph.D., a post-doctoral research assistant in Bae's lab and first author on the paper. "Lymphocyte delivery of nanoparticles allows a wide range of medicines to be applied through this method."
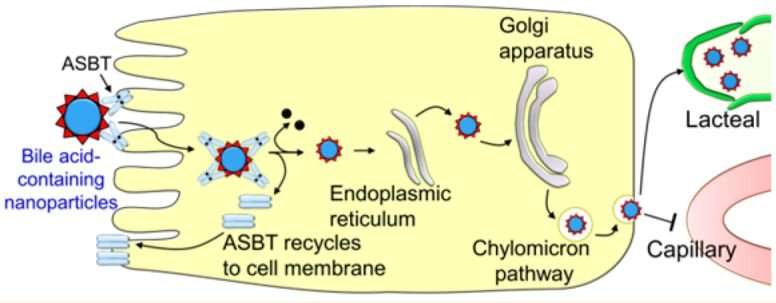
Without this chemical cloak, only seven percent of nanoparticles are absorbed and enter the blood stream. With this new technique, bioavailability increased seven-fold. Bae notes that it takes about one to ten hours for the nanoparticles to appear in the bloodstream.
Bae and his colleagues found nanoparticle size matters. They fed rodents oral nanoparticles in two sizes (100 or 250 nm) at doses ranging from 1 to 20 mg/kg. Surprisingly, larger nanoparticles were not less well absorbed. Dose, however, did not affect the uptake of nanoparticles into the body.
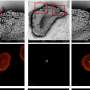
To monitor the nanoparticle movement, the researchers affixed a red fluorescence tag on the treated particles and watched the particles circulate through the body.
Nanoparticles are tiny—ten thousand times smaller than the head of a pin. In medicine, researchers design these particles to seek out diseased cells for direct treatment, reducing the damage to risk of damage to healthy cells. Researchers have long sought a way to deliver an oral dose of nanoparticles to make these treatments more accessible to patients.
Bae notes that this work is still at the preliminary stages and more work is needed to move the results from animal studies to clinical trials. As a proof of concept, the researchers used polystyrene nanoparticles that are not appropriate for clinical use because the particles are not dissipated or excreted from the body.
"This is basic research with broad future applications," Bae said. "Our work is a stepping stone."
More information: "Oral Nanoparticles Exhibit Specific High-Efficiency Intestinal Uptake and Lymphatic Transport" ACS Nano (2018). pubs.acs.org/doi/abs/10.1021/acsnano.8b04315
Journal information: ACS Nano
Provided by University of Utah