Researchers find blood vessel endothelial cells stop more nanoparticles than the liver
Nanoparticles that transport medicines to a specific part of the human body are usually broken down in the liver prematurely. Jeroen Bussmann from Leiden University has discovered a new method to prevent this from happening. Publication in ACS Nano.
In nanotherapy, particles measuring between a nanometer and a micrometer are used to deliver medicines to specific locations in the body, for example to destroy tumours with far fewer side-effects than traditional chemotherapy. A recurrent problem in developing nanotherapy is that the liver often breaks down the nanoparticles prematurely. Consequently, the particles only rarely reach their intended destination. To date, researchers believed this was the work of clean-up cells – so-called Kupffer cells – in the liver.
Cells from blood vessel walls
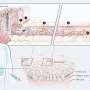
In joint research carried out with the Hubrecht Institute and the University of Basel, Jeroen Bussmann, chemical biologist at Leiden University, discovered that cells in the blood vessel walls of the liver (endothelial cells) often play a much greater role in this process than previously thought. Proteins on the surface of these cells recognise the nanoparticles and eliminate them. Blocking these proteins means that the endothelial cells will no longer recognize the nanoparticles, which then remain in the blood for longer. This is crucial if medicines are to be reach their intended targets in the body.
Tracking nanoparticles
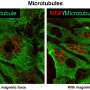
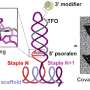
Bussmann used zebrafish larvae for his research. "The advantage of using these larvae is that they are transparent, so we can follow the nanoparticles using a microscope in the blood vessels," he explains. Bussmann blocked the endothelial cells by giving the zebrafish larvae a special polymer (a long, interlinked molecule). "When this polymer binds to the proteins on the endothelial cells, they no longer recognise the nanoparticles," he explains.
The other clean-up cells in the liver (Kupffer cells) mainly recognise particles larger than 100 nanometers. The idea was that by using smaller nanoparticles in combination with the special polymer, no cells in the liver would still be able to cause the removal of the nanoparticles. This worked: particles administered in this way remain in the blood stream without being broken down.
Blood vessel cells swallow up nanoparticles
The point in time when Bussmann was certain that the endothelial cells had actually ingested the nanoparticles, was when he administered nanoparticles containing a toxic substance to the fish larvae: this substance only acts within cells and not outside them. So, when only the endothelial cells died, he knew that this was because they had ingested the nanoparticles.
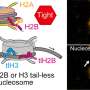
Using the zebrafish larvae, Bussmann also discovered precisely which protein in the endothelial cells binds to the particles, namely Stabilin-2. Removing the gene for Stabilin-2 also resulted in much lower breakdown of the nanoparticles. Bussmann now aims to develop a molecule that binds specifically to Stabilin-2. It will then be possible to inhibit the breakdown function of the cells highly specifically, without the liver losing part of its natural function.
Delivering medicines to cells
Bussmann also wants to explore how exactly the protein binds to the particles and how the endothelial cells subsequently ingest them. "We want to understand every step in the process so that we can ultimately produce nanoparticles that can deliver medicines not only to the liver but to every type of cell in the body."
The article has been published in ACS Nano.
More information: Frederick Campbell et al. Directing Nanoparticle Biodistribution through Evasion and Exploitation of Stab2-Dependent Nanoparticle Uptake, ACS Nano (2018). DOI: 10.1021/acsnano.7b06995
Journal information: ACS Nano
Provided by Leiden University