Scientists design nano-sized drug transporter to fight disease
Scientists seeking to improve cancer treatments have created a tiny drug transporter that maximizes its ability to silence damaging genes by finding the equivalent of an expressway into a target cell.
The transporter, called a nanocarrier, is a lipid-based structure containing a piece of RNA. Lipids are fatty molecules that help maintain the structure of cell membranes.
The RNA segment encased in the carrier sets off a process to silence genes, rendering the genes unable to produce proteins that lead to disease or other health problems.
Though the main component of the carrier resembles existing and previously studied transporters, Ohio State University scientists have attached specific helper molecules to the carrier's surface that their research suggests can enhance the transporter's effectiveness.
By finding the pathways that are equivalent to highways, vs. pathways similar to slower local routes, to get into the cells, the carriers then spend more time in the parts of the cells where they can dissolve and deposit the RNA segments. These segments, called small interfering RNA or siRNA, then can silence target genes for a prolonged period of time.
Recent studies suggest that the Ohio State-designed nanocarrier allows for a six-fold decrease in production of target proteins compared to the gene silencing effects resulting from the use of previously tested transporters.
"We have designed a different nanocarrier formulation and demonstrated that this formulation can affect the cellular entry pathway, which in turn affects how long the siRNA is exposed to the main body of the cell," said Chenguang Zhou, a graduate student in pharmaceutics at Ohio State and lead author of the study. "More of that exposure equals better and longer gene silencing."
The research was selected for a 2011 American Association of Pharmaceutical Scientists (AAPS) Innovation in Biotechnology Award. Zhou was invited to present the work at the recent AAPS National Biotechnology Conference.
The role of siRNA in cells has been established as an important gene-regulation mechanism that has the potential to protect cells against invaders, such as viruses, or to diminish the activity of oncogenes that cause cancer. But harnessing siRNA's protective properties for therapeutic purposes has been difficult, partly because siRNA is too big and complex to travel through the gastrointestinal system or bloodstream. It also has a negative charge, as do most cell membranes, meaning that unless it is naturally generated inside a cell, it cannot penetrate cells by itself.
Other research groups have developed lipid-based nanocarriers. The nanocarrier that Zhou and his colleagues have designed, however, uses a different method – it has a special compound on the surface that helps it slip more easily into the cell.
In all cases, a synthetic form of siRNA – one that is specifically related to a target gene – is manufactured to mimic the pieces of RNA that exist in nature. The siRNA is then encapsulated inside the nanocarrier, which functions as an siRNA delivery device into target cells.
In experiments in cells comparing the effects of traditional nanocarriers and Zhou's carrier, called a SPANosome, the researchers found that siRNA delivered by the SPANosome was about six times more effective at silencing the target gene activity than was the siRNA transported by traditional carriers. The Ohio State carrier reduced the associated protein production by 95 percent, compared to a 70.6 percent reduction in proteins resulting from the use of the traditional carrier.
The researchers then set out to find out why their carrier was so effective.
They knew, based on previous research, that to perform its role, siRNA must escape from a compartment inside a cell to maximize its exposure to the main body of the cell. It also must avoid another specific part of the cell where outsiders are degraded and fall apart. This whole process is called pharmacokinetics.
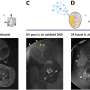
To observe this activity, the scientists used sophisticated fluorescent imaging techniques to detect how effective the siRNA was at different time points after it was introduced to cells via different types of carriers. They found that four hours after introduction to liver cancer cells, the siRNA transported by the SPANosome had 3.5 times more exposure to the cell body than did siRNA transported by more traditional carriers.
"We saw a correlating increase of 3.5 times more gene silencing activity," Zhou said. "The reason you want to study pharmacokinetics is because you want to find the exposure and response relationship. The reason the SPANosome is more effective is because it allows for increased exposure of siRNA to the main part of the cell."
Because siRNA can occur naturally in every cell, nanocarriers used to deliver siRNA for therapeutic purposes must be designed so that they penetrate only target cells, such as tumor cells or liver cells, to silence specific genes related to disease. The researchers used additional imaging techniques to track how their carrier finds its target cells.
And this is where the highway concept came into play. Nanocarriers have essentially three possible pathways into the cell – two that are equivalent to highways and one that is more similar to a slower, local route. The SPANosome, because of its design, uses the highway pathways to enter liver cancer cells, reducing its chances of getting sent to parts of the cell where it will be broken into pieces.
Zhou and colleagues are collaborating with medical and biotech industry researchers to further test the SPANosome as a potential vehicle to deliver drugs for cancer treatment, especially in liver cancer.
Provided by The Ohio State University