This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Blood stem cells found to not be in charge in an emergency
As long as we are healthy, our body keeps the number of blood and immune cells largely constant. However, any infection or other disorder that increases cell consumption results in cell loss, which must be replaced as quickly as possible to keep the immune system fully functional.
During embryonic development, blood stem cells in the bone marrow give rise to all types of mature blood cells. "Therefore, it has long been presumed that the loss of blood and immune cells in emergency situations is signaled to the blood stem cells, which are stimulated to divide much faster than usual to immediately provide replacement," says Hans-Reimer Rodewald of DKFZ.
Blood stem cells can divide into a daughter cell, which remains a stem cell, and a second daughter cell, which continues to develop. These developing daughter cells first give rise to so-called multipotent progenitor cells, which are capable of differentiate into any type of blood cell.
"Until now, we didn't know exactly whether it is actually the blood stem cells that provide regeneration in an emergency—or whether the progenitor cells take over this job," explains immunologist Katrin Busch, one of the first authors of the current paper.
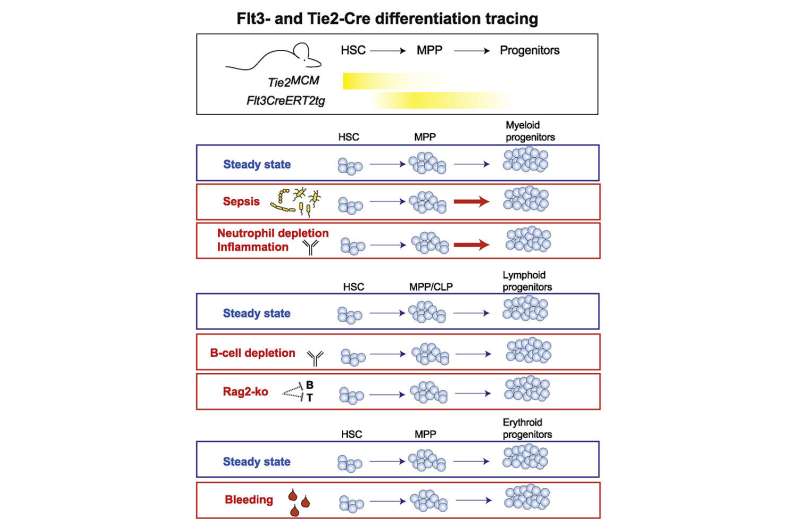
Rodewald's team, in collaboration with Thomas Höfer's research group, also at DKFZ, has now been able to investigate this question in mice. To this end, the researchers used genetic markers that were incorporated into the blood stem cells and that can be traced through all further developmental steps in their cell progeny.
If the mice were infected with bacteria, they developed a systemic inflammation. As expected, the labeled blood stem cells reacted with cell division—which, however, did not result in an increased number of differentiated blood cells. In addition, the stem cells intensified transcription, but this primarily affected those genes that are associated with their self-renewal.
Thus, the blood stem cells themselves are apparently not in charge of replenishing mature blood cells. This was true not only for bacterial infections, but also for other stressful health conditions such as anemia or a deficiency of various types of immune cells.
However, the situation was quite different when the population of multipotent progenitor cells was equipped with the genetic marker: After about eleven days, the number of different labeled white blood cells that emerged from the multipotent progenitor cells increased significantly in the bacterially infected mice.
"Having the progenitor cells do this task has several advantages: It speeds up the process, because differentiation from stem cells is a fairly slow process. In addition, there are significantly more progenitor cells than stem cells—this also helps to ensure that sufficient mature blood cells are available quickly," explains Höfer.
"We also interpret the result as a possible protective mechanism of the blood stem cells, perhaps in order to avoid being exhausted by recurrent infections in the course of life," adds Rodewald.
A few years ago, scientists from Rodewald's and Höfer's lab had already demonstrated that, contrary to common expert opinion, pluripotent progenitor cells also play a major role in maintaining the number of blood cells under normal healthy conditions.
More information: Hans-Reimer Rodewald, Flt3- and Tie2-Cre tracing identifies regeneration in sepsis from multipotent progenitors but not hematopoietic stem cells, Cell Stem Cell (2023). DOI: 10.1016/j.stem.2022.12.014. www.cell.com/cell-stem-cell/fu … 1934-5909(22)00498-2
Journal information: Cell Stem Cell
Provided by German Cancer Research Center