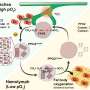
A novel antibiotic idea: Preventing bacterial stickiness
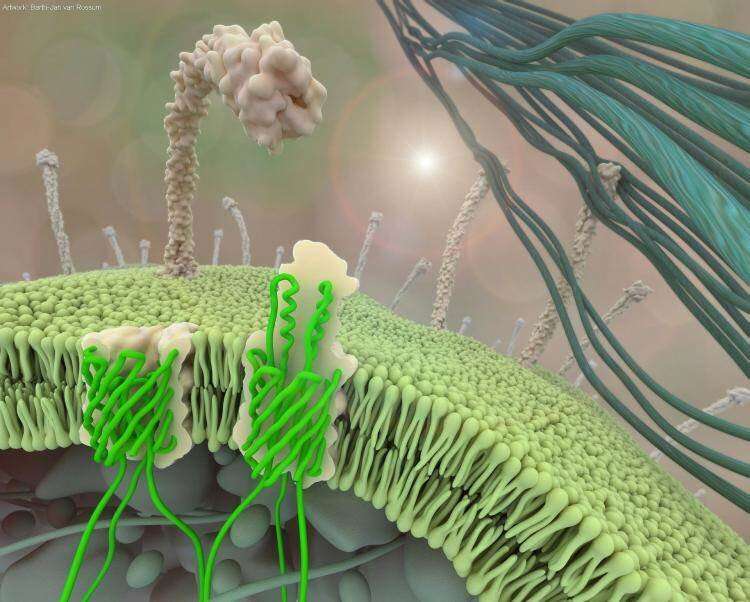
Researchers within the Dirk Linke group in the Department of Biosciences, University of Oslo, are proposing a new method to fight the bacterium Yersinia enterocolitica, which causes severe diarrhea in an estimated 10 million children each year—mainly in the world's poorest countries. This strategy should give the pharmaceutical industry a new weapon in the fight against antibiotic-resistant bacteria, which is a major problem in both rich and poor countries. It could also be used to inhibit bacteria from binding to prostheses and implants, forming large colonies called biofilms.
In addition, the researchers see several possible applications in industry, such as shipping and the aquaculture, where bacteria and biofilms can be a big problem. It is all about attacking the bacteria in a completely new way, the researchers say.
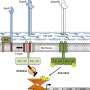
"For bacteria to cause an infection, they must first attach to a surface, such as the cells in our body. The same applies when bacteria form biofilms—they must attach themselves to a surface. Bacteria have evolved a number of techniques that make this possible," Professor Dirk Linke says.
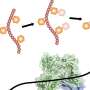
One of these tricks is to produce very sticky molecules called adhesins that cover the bacterial cell surface. Thus, a bacterium can use the adhesins to attach to a substrate, or to make a biofilm by attaching itself to other bacteria. "By interfering with the production of the adhesins, we can potentially fight infections already in the start-up phase—that is, before the symptoms occur," postdoc Marcella Orwick-Rydmark says.
Adhesins are long, hair-like proteins with a sticky tip. These hairs can grow so tightly that they more or less cover the bacterial cell surface, as if the bacteria were covered in Velcro. Dirk Linke and his team of researchers, including Marcella Orwick-Rydmark and Daniel Hatlem, now describe how adhesins are produced inside the bacterial cells and transported to the surface. They have also studied how it is possible to block this process. The findings are published in Molecular Microbiology.
Blocking the transport of adhesins to the cell's surface will in practice cause the bacteria to lose their ability to attach to anything, make biofilms or cause infections, the researchers believe.
Long-term work
Ten years of hard work lies behind this new discovery. The Yersinia adhesins studied in this particular project were discovered nearly 10 years ago, and it was within the last two years that Dirk Linke's group has discovered how they were transported to the cell surface, and how they can genetically block this process.
The researchers believe that these discoveries are far reaching, as adhesins are important in other diseases such as tuberculosis, plague and cystic fibrosis. Artificial hips and other surgical implants can also be covered by biofilms, which can cause such serious infections and the eventual removal of implants, which is painful and expensive. It is also relatively common for people with urinary tract infections to develop biofilm-like structures within the cells along the urinary tract, which can act as a reservoir for new infections.
"We therefore believe that this is a major advance when we have now shown how we can block the production of adhesins in a bacterium. But I want to emphasize that it will still take time before we can present a new drug. We may need another five to 10 years of continued research and development work," says Linke.
Mutations prevent the formation of adhesin molecules
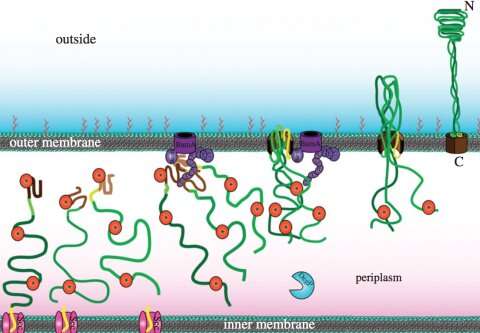
The researchers describe how adhesin proteins are produced by Yersinia enterocolitica. They have also studied which parts of the protein are central during transport from the inside of the bacterium to the cell membrane. In addition, the researchers have introduced mutations that block this process.
"We have come a long way in understanding which part of the adhesin protein can be blocked by mutations. The next step is to develop a molecule that binds to that part of the protein, and this can become a future drug. This then becomes a fairly classic development project, which we have good opportunities to carry out here at UiO and the Norwegian Center for Molecular Medicine," says Linke.
Marcella Orwick-Rydmark emphasizes that the bacteria do not die if they are exposed to a drug that only destroys the adhesin production. This can actually be an advantage because the bacteria are less likely to develop new defense mechanisms through evolution. A bacterium that is unable to produce adhesin can still be able to reproduce.
"No drugs have been developed previously that attack these adhesin molecules. This means that the bacteria cannot use any of the old techniques they have developed to protect themselves against antibiotics," she adds. Additionally, drugs that target adhesin molecules could also be used in combination with classical antibiotics, leading to even better outcomes for someone with an infection.
Biofilms are everywhere
The UiO researchers have already received considerable feedback from other interested researchers. During the coming months, they will, among other things, present the new findings at several scientific conferences.
Biofilms are more widespread than most people might think about. For example, the rings that form in toilets and bathtubs are examples of biofilms, as well as the plaque on teeth. Biofilms also exist practically everywhere in nature where there is a solid surface surrounded by water. You have probably noticed that stones in running water can be very slippery—this is due to biofilms that contain many bacterial species. But these are the not the biofilms that Linke, Hatlem, and Rydmark are planning to target—yet.
More information: Nandini Chauhan et al. Insights into the autotransport process of a trimeric autotransporter, Yersinia Adhesin A (YadA), Molecular Microbiology (2019). DOI: 10.1111/mmi.14195
Journal information: Molecular Microbiology
Provided by University of Oslo