CRISPR/Cas9 gene editing scissors are less accurate than we thought, but there are fixes

CRISPR gene editing technology is revolutionising medicine and biology. This technique allows scientists to edit DNA with more precision and greater ease than previous gene editing technology.
But a new study has called into question the precision of the technique.
The hope for gene editing is that it will be able to cure and correct diseases. To date, many successes have been reported, including curing deafness in mice, and in altering cells to cure cancer.
Some 17 clinical trials in human patients are registered testing gene editing on leukaemias, brain cancers and sickle cell anaemia (where red blood cells are misshaped, causing them to die). Before implementing CRISPR technology in clinics to treat cancer or congenital disorders, we must address whether the technique is safe and accurate.
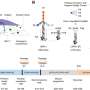
How does CRISPR work again?
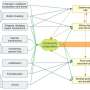
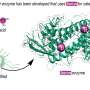
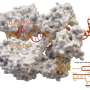
CRISPR technology utilises molecular scissors (a bacteria enzyme called "Cas9") to cut the DNA we want to target, and then we can paste DNA in to replace what we have removed. Cas9 recognises a specific segment of DNA among the entire human genome by utilising a guide, something like a map, that is linked to Cas9.
Cas9 can persist in the body for several hours to several weeks. While it remains in the body, Cas9 can cut and paste other segments of DNA ("off targets") or the targeted segment of DNA over and over ("on target").
What the new study found
A study published today in Nature Biotechnology explores the accuracy of the Cas9 scissors. Scientists at the Sanger Institute at Cambridge, UK sought to determine whether Cas9's cut and paste process is accurate enough to be safely used in humans for treating disease.
To answer this important question, they examined in detail the DNA segments in mouse embryonic stem cells and human cells near the segment that was cut to see if they were affected.
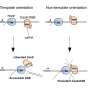
They found that after the DNA was repaired (new DNA pasted into the "cut" segment), the scissors continued to cut the DNA over and over again. They found significant areas near the cut site where DNA had been removed, rearranged or inverted.
If a fragment of DNA is removed or inverted (the genes switched around), the gene modification could be dangerous, and even lead to disease. While this seems scary, this could potentially be overcome using new sequencing technologies.
Can we use different scissors?
There are a few options for getting around this problem. One option is to isolate the cells we wish to edit from the body and reinject only the ones we know have been correctly edited.
For example, lymphocytes (white blood cells) that are crucial to killing cancer cells could be taken out of the body, then modified using CRISPR to heighten their cancer-killing properties. The DNA of these cells could be sequenced in detail, and only the cells accurately and specifically gene-modified would be selected and delivered back into the body to kill the cancer cells.
While this strategy is valid for cells we can isolate from the body, some cells, such as neurons and muscles, cannot be removed from the body. These types of cells might not be suitable for gene editing using Cas9 scissors.
Fortunately, researchers have discovered other forms of CRISPR systems that don't require the DNA to be cut. Some CRISPR systems only cut the RNA, not the DNA (DNA contains genetic instructions, RNA convey the instructions on how to synthesise proteins).
As RNA remains in our cells only for a specific period of time before being degraded, this would allow us to control the timing and duration of the CRISPR system delivery and reverse it (so the scissors are only functional for a short period of time).
This was found to be successful for dementia in mice. Similarly, some CRISPR systems simply change the letters of the DNA, rather than cutting them. This was successful for specific mutations causing diseases such as hereditary deafness in mice.
In short, before using CRISPR clinically, we still have a lot to learn about the effects of Cas9 scissors in the cells.
Provided by The Conversation
This article was originally published on The Conversation. Read the original article.![]()