Sugar sponges sop up and release glucose as needed
Many diabetes patients must inject themselves with insulin, sometimes several times a day, while others take medications orally to control blood sugar. The injections, as well as the side effects from both regimens, can be painful. Now, one team reports in the Journal of the American Chemical Society progress toward an insulin-free diabetes treatment that requires fewer injections.
According to the U.S. Centers for Disease Control and Prevention, current trends predict that one in three adults in the U.S. will have diabetes by 2050. Treatments include insulin injections, which can be painful. In addition, the injections can involve different types of insulin—a slow-acting one before bed or a fast-acting one before meals—which can be confusing. Pills are not much better, as patients sometimes forget to take them. Both drugs and injections can have various side effects, including nerve damage, infections and insulin resistance. Non-invasive insulin-dependent systems that include hydrogels and polymers have developed in the laboratory, but they also can trigger these complications. So Jianzhong Du and colleagues wanted to develop a method that would be easy to use and that would avoid side effects.
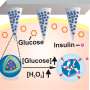
The researchers nicknamed their treatment the "sugar sponge." It's an injected lectin-coated polymer vesicle that sopped up and bound glucose when glucose levels were high, and released the sugar when its concentrations were low in laboratory tests. They also tested the sponge in mice with type-I diabetes, and within two days, they saw antidiabetic effects. The researchers say that the sponge could one day serve as a treatment for either type-I or type-II diabetes.
More information: Yufen Xiao et al. Sugar-Breathing Glycopolymersomes for Regulating Glucose Level, Journal of the American Chemical Society (2017). DOI: 10.1021/jacs.7b03219
Abstract
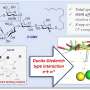
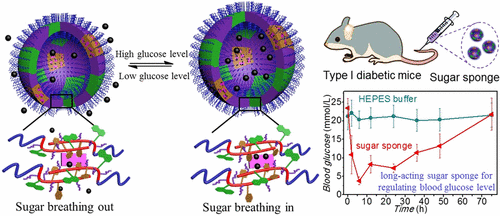
Diabetes mellitus is a chronic, life-threatening illness that affects people of every age and ethnicity. It is a long-term pain for those who are affected and must regulate their blood glucose level by frequent subcutaneous injection of insulin every day. Herein, we propose a noninsulin and antidiabetic drug-free strategy for regulating blood glucose level by a nanosized "sugar sponge" which is a lectin-bound glycopolymersome capable of regulating glucose due to the dynamic recognition between the lectin and different carbohydrates. The glycopolymersome is self-assembled from poly(ethylene oxide)-block-poly[(7-(2-methacryloyloxyethoxy)-4-methylcoumarin)-stat-2-(diethylamino)ethyl methacrylate-stat-(α-d-glucopyranosyl)ethyl methacrylate] [PEO-b-P(CMA-stat-DEA-stat-GEMA)]. The lectin bound in the glycopolymersome has different affinity for the glucose in the blood and the glucosyl group in the glycopolymersome. Therefore, this sugar sponge functions as a glucose storage unit by dynamic sugar replacement: The lectin in the sugar sponge will bind and store the glucose from its surrounding solution when the glucose concentration is too high and will release the glucose when the glucose concentration is too low. In vitro, this sugar-breathing behavior is characterized by a remarkable size change of the sugar sponge due to the swelling/shrinkage at high/low glucose levels, which can be used for blood sugar monitoring. In vivo, this sugar sponge showed an excellent antidiabetic effect for type I diabetic mice within 2 days upon one dose, which is much longer than traditional long-acting insulin. Overall, this concept of "controlling sugar levels with sugar" opens new avenues for regulating the blood glucose level without the involvement of insulin or other antidiabetic drugs.
Journal information: Journal of the American Chemical Society
Provided by American Chemical Society