Study finds specialized bacterial cells found in the gut produce steroid hormones
The human gut is home to trillions of bacteria, many of which play an important role in helping the body strike a healthy balance. In the gut, bacteria are involved in the synthesis of vitamins, as well as metabolizing bile acids, cholesterol and other chemicals found in the body that are not typically produced by the body. Bacteria in the gut also can produce a plethora of new hormones.
With all its metabolic activities, it comes as no surprise that some researchers view the gut as an organ.
Recently, a team of researchers at Virginia Commonwealth University provided additional evidence that the bacteria found living inside the human gut may represent an endocrine organ. For example, the VCU team discovered that specialized gut bacterial cells produce steroid hormones – much like specialized cells in the pancreas produce the endocrine molecule insulin.
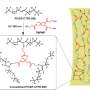
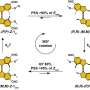
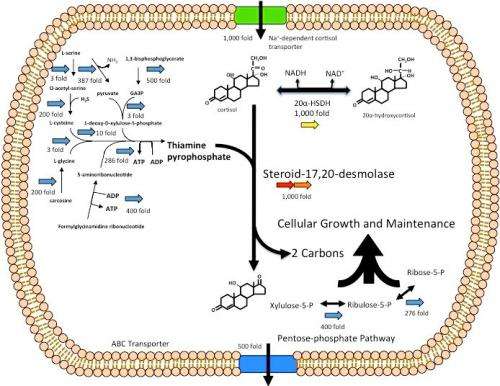
In a study featured on the cover of the September 2013 print issue of the Journal of Lipid Research, researchers used advanced technology to identify genes of a bacterium called Clostridium scindens. C. scindens is found in the gut and encodes for a class of enzymes that cause a profound change in the structure of cortisol, a hormone produced by the adrenal gland. Small changes in shape and structure of steroids can have profound effects on the human body.
"Finding the genes involved in production of androgens from cortisol by gut bacteria is a big step toward figuring out what role these bacteria and the androgens play in human health,"said lead authorJason M. Ridlon,Ph.D.,affiliate assistant professor in the Department of Microbiology and Immunology in the VCU School of Medicine.
While it is known that these androgens re-enter the bloodstream from the gut, the implications of this are not completely clear, Ridlon said.
One possibility is that these androgens may enter the male prostate, which presses against the colon, he said. Exposure of this nature that takes place during the course of many years could result in disease, such as prostate cancer, in some individuals.
"Prostate, as well as colon, cancer is related to diet with risk increasing with a highfat, high animal protein diet," Ridlon said. "This same diet favors the bacteria that convert these stress hormones into androgen. The androgen produced by these bacteria may pass through the colonic wall into the prostate and represent one environmental factor in the etiology of the disease. This is an avenue that is worth exploring."
"Furthermore, the androgen produced by this one bacterium can be further modified by other gut microbes yielding a cocktail of androgens, which may affect the prostate or perhaps other tissues of the body. We may also find that these molecules are part of the normal crosstalk between microbe and human and may be part of our normal physiology. We are keeping an open mind here and letting the data tell us the significance of this interesting phenomenon."
Moving forward, the team will continue their investigation of the bacterium with the hopes of uncovering additional genes.
"It turns out that the bacterial equivalent of fraternal twins of this bacterium is capable of further modifying the androgen produced," Ridlon said. "These steroids seem to 'ping-pong' from one bacterium to another and new variants are made."
The team is in the process of collecting the steroids that these bacteria make and testing their effects on human cells so that they can determine any potential effects they have on the human body.
The study is titled "Clostridium scindens: a human gut microbe with a high potential to convert glucocorticoids into androgens."
More information: www.jlr.org/content/54/9/2437.long
Journal information: Journal of Lipid Research
Provided by Virginia Commonwealth University