Formula-feeding linked to metabolic stress and increased risk of later disease

New evidence from research suggests that infants fed formula, rather than breast milk, experience metabolic stress that could play a part in the long-recognized link between formula-feeding and an increased risk of obesity, type 2 diabetes and other conditions in adult life. The study appears in ACS' Journal of Proteome Research.
Carolyn Slupsky and colleagues explain that past research showed a link between formula-feeding and a higher risk for chronic diseases later in life. Gaps exist, however, in the scientific understanding of the basis for that link. The scientists turned to rhesus monkeys, stand-ins for human infants in such research, that were formula-fed or breast-fed for data to fill those gaps.
Their analysis of the monkeys' urine, blood and stool samples identified key differences between formula-fed and breast-fed individuals. It also produced hints that reducing the protein content of infant formula might be beneficial in reducing the metabolic stress in formula-fed infants. "Our findings support the contention that infant feeding practice profoundly influences metabolism in developing infants and may be the link between early feeding and the development of metabolic disease later in life," the study states.
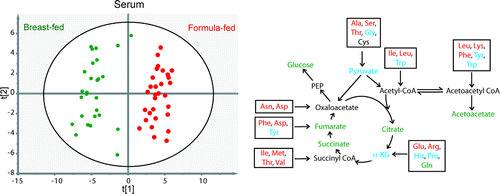
The article is titled "Early Diet Impacts Infant Rhesus Gut Microbiome, Immunity, and Metabolism."
More information: Early Diet Impacts Infant Rhesus Gut Microbiome, Immunity, and Metabolism, J. Proteome Res., Article ASAP. DOI: 10.1021/pr4001702
Abstract
Epidemiological research has indicated a relationship between infant formula feeding and increased risk of chronic diseases later in life including obesity, type-2 diabetes, and cardiovascular disease. The present study used an infant rhesus monkey model to compare the comprehensive metabolic implications of formula- and breast-feeding practices using NMR spectroscopy to characterize metabolite fingerprints from urine and serum, in combination with anthropometric measurements, fecal microbial profiling, and cytokine measurements. Here we show that formula-fed infants are larger than their breast-fed counterparts and have a different gut microbiome that includes higher levels of bacteria from the Ruminococcus genus and lower levels of bacteria from the Lactobacillus genus. In addition, formula-fed infants have higher serum insulin coupled with higher amino acid levels, while amino acid degradation products were higher in breast-fed infants. Increases in serum and urine galactose and urine galactitol were observed in the second month of life in formula-fed infants, along with higher levels of TNFα, IFN-γ, IL-1β, IL-4, and other cytokines and growth factors at week 4. These results demonstrate that metabolic and gut microbiome development of formula-fed infants is different from breast-fed infants and that the choice of infant feeding may hold future health consequences.
Journal information: Journal of Proteome Research
Provided by American Chemical Society