New fluorescent biosensor reveals mechanism critical to immune system amplification
Using a new fluorescent biosensor they developed, researchers at Carnegie Mellon University have discovered how a key set of immune cells exchange information during their coordinated assault on invading pathogens. The immune cells, called dendritic cells, are harnessed by cancer vaccines and other therapeutics used to amplify the immune system. The finding, published online March 29 in the journal Angewandte Chemie, marks the first time that scientists have visualized how antigens are transferred in the immune system between dendritic cells.
"Knowing the mechanism behind what's going on in these dendritic cells — how they are talking to each other in order to amplify the immune response — is of fundamental significance," said Marcel P. Bruchez, associate professor of biological sciences and chemistry in the Mellon College of Science.
Dendritic cells are specialized immune cells that search for and capture foreign micro-organisms like bacteria, allergens or viruses. The cells engulf the invading organism and break it down into pieces. The dendritic cell then places these pieces, called antigens, on its cell surface.
When a dendritic cell presents antigens on its surface, it instructs other immune cells to multiply and scour the body in search of the harmful micro-organisms. Dendritic cells also can share antigens with other dendritic cells to boost immune cell activation. While scientists knew that antigens from one dendritic cell could show up in another dendritic cell, they didn't know how those antigens got there.
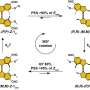
To determine the precise mechanism by which dendritic cells transfer antigens to each other, the research team used a new pH-biosensor developed at Carnegie Mellon's Molecular and Biosensor Imaging Center (MBIC). The biosensor is made up of two components: a fluorogen activating peptide (FAP), which is genetically expressed in a cell and tagged to a protein of interest, and a dye called a fluorogen, which either glows red or green depending on the pH level of its environment.
"All routes into the cell have characteristic pH profiles," Bruchez said. "Our pH-biosensor allows us to determine whether the tagged protein — in this case a surrogate antigen — is moving through neutral compartments into the cell, or through acidic compartments into the cell. Those sorts of things determine whether the antigen enters the cell through an active endocytic process, a phagocytic process, or a caveolar uptake process."
In the current study, researchers tagged a surrogate antigen on the surface of a dendritic cell with the FAP. They added the pH sensitive dye, causing the FAP antigen to glow green, an indication of a neutral pH. As the antigen and its bound dye passed to a separate dendritic cell, the antigen/FAP complex glowed red, indicating it used an acidic pathway to enter the new cell. This change in pH from neutral to acidic reveals that antigens are passed between cells through an active endocytic process.
"Once it's nibbled by the acceptor cell, the antigen goes through this endocytic pathway where it can potentially then be reprocessed and re-displayed on the surface of the receptor cell," Bruchez said.
The new biosensor's activity is novel, Bruchez said, because it binds to its target with nanomolar affinity, becomes fluorescently activated, and then is carried into the cell under endocytic conditions, reporting on the pH as it goes. The researchers are hopeful that this technology is the first in a platform of targetable environmental sensors. The current biosensor can read out pH, but this approach could be extended to measure calcium or other ion fluctuations in living cells. According to Bruchez, there are many ways that this basic chemical concept can be extended.
Provided by Carnegie Mellon University