Scientists show how shifts in temperature prime immune response
Researchers at The Scripps Research Institute have found a temperature-sensing protein within immune cells that, when tripped, allows calcium to pour in and activate an immune response. This process can occur as temperature rises, such as during a fever, or when it falls—such as when immune cells are "called" from the body's warm interior to a site of injury on cooler skin.
The study, recently published online ahead of print by Nature Chemical Biology, is the first to find such a sensor in immune cells—specifically, in the T lymphocytes that play a central role in activation of killer immune cells. The protein, STIM1, previously known as an endoplasmic reticulum (ER) calcium sensor, had been thought to be important in immune function, and now the scientists show it is also a temperature sensor.
"Temperature has a profound effect on all biological processes including immune responses, but surprisingly little is known about molecules in immune cells that sense temperature sifts," said the study's principal investigator, Scripps Research Professor Ardem Patapoutian. "Here we show that STIM1 senses temperature and has a profound impact on immune cells."
This is the second family of thermosensation molecules that the Patapoutian laboratory has uncovered. The team has isolated and characterized three of six members of the transient receptor potential (TRP) family of ion channels—the so-called thermoTRPs. "These proteins translate temperature, which is a physical stimulus, into a chemical signal—ions flowing into cells," said Patapoutian.
"ThermoTRPs mainly function in specialized sensory neurons that relay environmental temperature information to the brain."
In this study, the researchers turned to immune cells to look for temperature sensors. "Immune cells can experience dramatic temperature changes under either normal or pathophysiological conditions," said first author Bailong Xiao, a research associate in the Patapoutian laboratory. "The temperature drops significantly when, say, immune cells move from the 37 degree Celsius temperature of the spleen to skin, where it is normally 33 degrees. During fever, core body temperature can rise to 41 degrees." Scientists have discussed for decades whether fever is beneficial to the immune system. The researchers believe that identification of a molecular sensor of temperature within immune cells provides a novel avenue to address such questions mechanistically.
The research team, which included Bertrand Coste and Jayanti Mathur, also of the Patapoutian lab, found that STIM1 can be activated by heat with a high degree of temperature sensitivity. Both STIM1 and a plasma membrane pore-forming protein known as Orai1 have recently been identified as essential components of the so-called the calcium release activated calcium (CRAC) channel. But STIM1 had not been known to be heat sensitive until this research, according to Xiao.
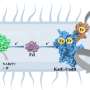
The process goes like this: STIM1 proteins are located on the ER, which is the organelle that stores calcium inside the cell. When a sudden change in temperature occurs, STIM1 proteins cluster together and translocate close to the plasma membrane. There, these clusters then can activate Orai1, which leads to the opening of the channel pore and an influx of calcium to activate the cell. Calcium is essential for a number of cellular functions, and, in immune cells, a sustained influx of calcium into these cells activates gene expression and cell proliferation. It turns the immune cell "on," Xiao said.
The function of STIM1 and Orai1 had already been known to be critical to immune function, Xiao said. Mutations in genes encoding either of the proteins lead to development of severe combined immunodeficiency (SCID), the so-called "bubble boy" disease characterized by a complete absence of immunity.
Given the relatively wide expression pattern of STIM1, the researchers suggest that STIM1 may also function as a temperature sensor in other tissues in addition to immune system, including skin, brain, skeletal muscle, and even in blood platelets, all of which could experience moderate but significant temperature changes. For example, temperature-induced STIM1-mediated calcium influx may help muscle cells remodel after exercise, Xiao explained. "We know that calcium is very important for skeletal muscle physiology and remodeling.
Temperature can rise in skeletal muscles when they are exercised."
The same principle may be working in blood platelets, where STIM1 is also found and plays important roles, he said. When platelets move to the skin surface to repair a cut, the change in temperature may activate STIM1, which can contribute to platelet activation, resulting in formation of a clot, Xiao said.
While sensing temperature is essential for survival and efficient metabolism, it is not clear yet if and how these findings can be clinically translated, said Patapoutian. "It is too early to make predictions on the implications of these findings, but STIM1 and Orai1 are of interest to the pharmaceutical industry given their role in immunodeficiency."
More information: Temperature-dependent STIM1 activation induces Ca2+ influx and modulates gene expression, Nature Chemical Biology (2011) doi:10.1038/nchembio.558
Abstract
Intracellular Ca2+ is essential for diverse cellular functions. Ca2+ entry into many cell types including immune cells is triggered by depleting endoplasmic reticulum (ER) Ca2+, a process termed store-operated Ca2+ entry (SOCE). STIM1 is an ER Ca2+ sensor. Upon Ca2+ store depletion, STIM1 clusters at ER–plasma membrane junctions where it interacts with and gates Ca2+-permeable Orai1 ion channels. Here we show that STIM1 is also activated by temperature. Heating cells caused clustering of STIM1 at temperatures above 35 °C without depleting Ca2+ stores and led to Orai1-mediated Ca2+ influx as a heat off-response (response after cooling). Notably, the functional coupling of STIM1 and Orai1 is prevented at high temperatures, potentially explaining the heat off-response. Additionally, physiologically relevant temperature shifts modulate STIM1-dependent gene expression in Jurkat T cells. Therefore, temperature is an important regulator of STIM1 function.
Provided by The Scripps Research Institute