Three-Dimensional Cell Culture: Making Cells Feel Right at Home
A team of Houston scientists has unveiled a new technique that uses magnetic nanobeads to levitate cells, allowing them to grow into three-dimensional structures. This technological leap from the flat Petri dish has the potential for significant impact on cancer research, where recent studies have demonstrated that cancer cells growing in two-dimensional sheets are not the optimal systems for studying potential anticancer agents. In fact, techniques for growing cells in three-dimensional structures could save millions of dollars in drug-testing costs.
Renata Pasqualini and Wadih Arap, of the University of Texas M.D. Anderson Cancer Center, and Thomas Killian, of Rice University, led this study, which was reported in the journal Nature Nanotechnology. Dr. Pasqualini is also a member of the University of Texas Health Science Center at Houston Physical Sciences-Oncology Center, one of 12 Centers funded by the National Cancer Institute to foster the development of innovative ideas and new fields of study based on knowledge of the biological and physical laws and principles that define both normal and tumor systems.
The three-dimensional technique is easy enough for most labs to set up immediately. It uses magnetic nanoparticles to levitate cells while they divide and grow. Compared with cell cultures grown on flat surfaces, the three-dimensional cell cultures tend to form tissues that more closely resemble those inside the body. "There's a big push right now to find ways to grow cells in three-dimensional because the body is three-dimensional, and cultures that more closely resemble native tissue are expected to provide better results for preclinical drug tests," said Dr. Killian. "If you could improve the accuracy of early drug screenings by just 10 percent, it's estimated you could save as much as $100 million per drug." For cancer research, the "invisible scaffold" created by the magnetic field goes beyond its potential for producing cell cultures that are more reminiscent of real tumors, which itself would be an important advance, added Dr. Arap.
To make cells levitate, the research team modified a combination of gold nanoparticles and engineered viral particles called "phage" that was developed in the lab of Drs. Arap and Pasqualini. This targeted "nanoshuttle" can deliver payloads to specific organs or tissues.
"A logical next step for us will be to use this additional magnetic property in targeted ways to explore possible applications in the imaging and treatment of tumors," Dr. Arap said.
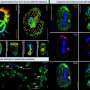
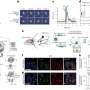
In the current study, the researchers added magnetic iron oxide nanoparticles to a gel that contains phage. When cells are added to the gel, the phage causes the particles to be absorbed into cells over a few hours. The gel is then washed away, and the nanoparticle-loaded cells are placed in a Petri dish filled with a liquid that promotes cell growth and division. By placing a coin-sized magnet atop the dish's lid, the researchers found that they could lift the cells off the bottom of the dish, concentrate them, and allow them to grow and divide while they were suspended in the liquid. In a key experiment using glioblastoma cells, the investigators found that cells grown in the three-dimensional medium produced proteins that were similar to those produced by gliobastoma tumors in mice, while cells grown in two dimensions did not show this similarity.
This work, which was supported in part by the National Cancer Institute, is detailed in a paper titled, "Three-dimensional tissue culture based on magnetic cell levitation." Investigators from Nano3D Biosciences, which has licensed this technology for commercial development, also participated in this study. An abstract of this paper is available at the journal's Web site.
Provided by National Cancer Institute