Researchers introduce rapid diagnostic test for Listeria

Researchers in the University of Georgia College of Engineering are developing a new way to detect potentially deadly Listeria contamination in food.
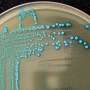
Listeriosis, an infection caused by eating food contaminated by the bacterium Listeria monocytogenes, can cause severe illness in pregnant women, newborns, the elderly and people with compromised immune systems. Listeria is the third leading cause of death from foodborne illness, or food poisoning, in the United States. An estimated 1,600 people get sick each year and about 260 die, according to the Centers for Disease Control and Prevention.
Currently, Listeria contamination in food products is identified only through molecular tests conducted in diagnostic laboratories on samples taken at specific control points during the manufacturing and distribution process. Although very accurate, this method requires significant processing time, transportation of samples, and expensive skilled labor and equipment.
In a new study published in the Journal of The Electrochemical Society, UGA researchers introduce a rapid diagnostic method based on electrochemical biosensing principles. Electrochemical biosensors are promising alternatives to molecular detection methods because of their ease of use, high specificity, sensitivity and low cost, according to the researchers.
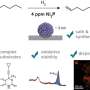
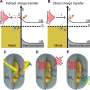
The UGA researchers use bacteriophages, viruses that infect and replicate within bacteria, as bioreceptors to identify L. monocytogenes using an electrochemical sensor.
"Bacteriophages are viruses that attack bacteria—they are very specific and will only attack their target," said Or Zolti and Baviththira Suganthan, two doctoral students in the College of Engineering who served as the study's lead authors. "We can take advantage of their specificity and make sure that only L. monocytogenes is detected on our sensor with little interference from biological agents."
Once the bacteriophages attract the target bacteria, they translate the biochemical information into an electrical signal that indicates the presence of contamination.
"Our approach is as good if not better than the competitive methods in the market in terms of their limits of detection," said Zolti.
Although the researchers have tested their system only in a laboratory setting, they are planning to apply what they've learned so far to actual contaminated food samples. If successful, the researchers could further optimize their sensors to meet the practical needs for early and rapid diagnosis in food industry.
"In our view, this sensor can be part of a food production line," said Zolti. "A manufacturer can use the sensor as a pre-screening tool to test for contamination."
Currently, the food industry sends samples of products to specialized laboratories that test the samples for contamination. This process can take from three days to two weeks, meaning products carrying Listeria may make it to grocery store shelves before the problem is identified.
"Our approach will allow food manufacturers to avoid recalls and find bacterial contamination within minutes on their production lines. This ability will also save lives and prevent contaminated products from reaching the shelves in supermarkets," said Zolti.
More information: Or Zolti et al, Electrochemical Biosensor for Rapid Detection of Listeria monocytogenes, Journal of The Electrochemical Society (2022). DOI: 10.1149/1945-7111/ac7a63
Journal information: Journal of The Electrochemical Society
Provided by University of Georgia