Genetic switch activates transformation of stem cells into heart muscle cells
The discovery of a genetic switch that triggers stem cells to turn into heart cells is a major step in finding treatment for damaged hearts.
Researchers from A*STAR and their colleagues in India have been investigating the molecular and genetic processes by which human embryonic stem cells differentiate into the body's many types of cells—in particular, cardiomyocytes, or heart muscle cells.
"The effort is underway globally to find ways to differentiate these stem cells into beating functional heart muscle cells so that they can be used for cell-based therapies to treat structural abnormalities," says Prabha Sampath, from the A*STAR Institute of Medical Biology.
In this study, researchers used a method called transcriptome profiling, which examines the activity of a wide range of genes in a cell, to determine which are more active when human embryonic stem cells differentiate into heart cells.
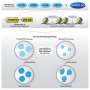
Two particular genes, NR2F2 and EZH2, show increased expression during the differentiation process. The proteins that these genes code for suppress the activity of another gene called OCT-4, which is responsible for keeping stem cells in their undifferentiated state.
"NR2F2 recruits EZH2 to gene OCT-4, and potentially suppresses its expression, propelling the cells towards differentiation," Sampath says. "With the down-regulation of this gene, the cells start differentiating into cardiomyocytes."
The NR2F2 protein has not previously been linked to cardiac differentiation, but mutations in the NR2F2 gene have been known to cause the development of a type of congenital heart defect. "While it's unlikely to be the only mechanism involved in the differentiation of stem cells into cardiac cells, it's an important step in the process", says Mohsin Bin Bashir, also from the Institute of Medical Biology. "If we can understand how a stem cell becomes a cardiomyocyte, we have more chance of creating these cells in a controlled fashion."
That process could also be used in reprogramming adult stem cells, where normal cells are taken from a patient, reprogrammed back into their stem cell state, then differentiated into whatever cell type is needed for treatment.
"You can convert them into cardiomyocytes and put them back into the patient, and one of the advantages with that [process is that] there would be no immune rejection because these cells come from the patient themselves," Bashir says.
More information: Varsha Pursani et al. Genetic and Epigenetic Profiling Reveals EZH2-mediated Down Regulation of OCT-4 Involves NR2F2 during Cardiac Differentiation of Human Embryonic Stem Cells, Scientific Reports (2017). DOI: 10.1038/s41598-017-13442-9
Journal information: Scientific Reports