Tissue engineers recruit cells to make their own strong matrix
Imitation may be the sincerest form of flattery but the best way to make something is often to co-opt the original process and make it work for you. In a sense, that's how scientists at Brown University accomplished a new advance in tissue engineering.
In the journal Biomaterials, the team reports culturing cells to make extracellular matrix (ECM) of two types and five different alignments with the strength found in natural tissue and without using any artificial chemicals that could make it incompatible to implant.
ECM is the fibrous material between cells in tissues like skin, cartilage, or tendon that gives them their strength, stretchiness, squishiness, and other mechanical properties. To help patients heal wounds and injuries, engineers and physicians have strived to make ECM in the lab that's aligned as well as it is when cells make it in the body. So far, though, they've struggled to recreate ECM. Using artificial materials provides strength, but those don't interact well with the body. Attempts to extract and build upon natural ECM have yielded material that's too weak to reimplant.
The Brown team tried a different approach to making both collagen, which is strong, and elastin, which is stretchy, with different alignments of their fibers. They cultured ECM-making cells in specially designed molds that promoted the cells to make their own natural but precisely guided ECM.
"What we hypothesized is that the cells are making it the same way they do in the body, because we're starting them in a more natural environment," said lead author Jacquelyn Schell, assistant professor (research) of molecular pharmacology, physiology and biotechnology. "We're not adding exogenous materials."
The strategy built on the insight that when cells clump together and grow in culture, they pull on each other and communicate as they would in the body, Schell said. The molds therefore were made from agarose so that cells wouldn't stick to the sides or bottom. Instead they huddled together.
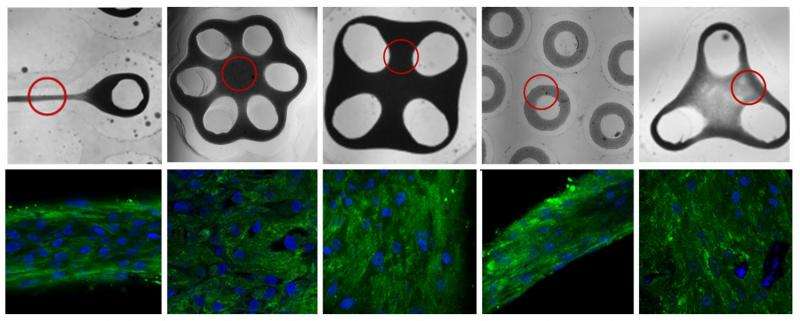
To guide ECM growth in particular alignments, the researchers used molds with very specific shapes, often constrained by pegs the cells had to grow around. For instance, to make a rod with collagen fibers aligned along its length (like a tendon) they cultured chondrocyte cells in a dog bone-shaped mold with loops on either end. To make a skin-like "trampoline" of elastin, where the ECM fibers run in all directions, they cultured fibroblast cells to grow in an open area suspended at the center of a honeycomb shape.
"The placement of the pegs that this group of cells wraps itself around and then exerts force on each other is what dictates their alignment and the direction of the ECM they are going to synthesize," said senior author Jeffrey Morgan, professor of medical science and engineering and co-director of Brown's Center for Biomedical Engineering. "That's a new ability to control the cells' synthesis of extracellular matrix."
After the researchers grew various forms of ECM, they did some stress testing. They took the dog bone-shaped tissues to the lab of Christian Franck, assistant professor of engineering, and together made precise measurements of the tissue strength under the force of being pulled apart. The measurements confirmed the self-assembled tissue was about as strong as that found in some of the body's tissues, such as skin, cartilage or blood vessels.
The team's next goal is to identify a prospective clinical application, Morgan said. The lab will pursue the needed testing to see if this new way of growing ECM can help future patients.
Journal information: Biomaterials
Provided by Brown University