Toward 24-7 glucose monitoring to help manage diabetes
Nearly half a million people with diabetes end up in emergency rooms around the U.S. every year due to the seizures and other consequences of dropping or spiking blood-sugar levels associated with the disease. To help prevent serious complications, scientists have now developed a new glucose-sensing protein that could one day be part of an implantable, 24-7 monitoring device. They describe the protein in the journal ACS Chemical Biology.
Sylvia Daunert and colleagues note that scientists have been working on new ways to track glucose levels. Most patients with diabetes do this by using a glucose meter. They prick a finger with a tiny needle to draw blood, which they apply to a test strip inserted into the meter. It provides a reading of the level at that moment. But glucose levels change throughout the day, so many readings are needed. That's not always convenient, and some people find that pricking their finger is painful. As a result, many patients don't test their blood as often as they should, risking complications such as seizures. For more continuous monitoring, some patients use implantable devices that measure blood-sugar as often as once a minute, but they have drawbacks. They are expensive, can only be used for up to a week and are not as reliable as conventional meters. Daunert's team set out to improve upon these limited options.
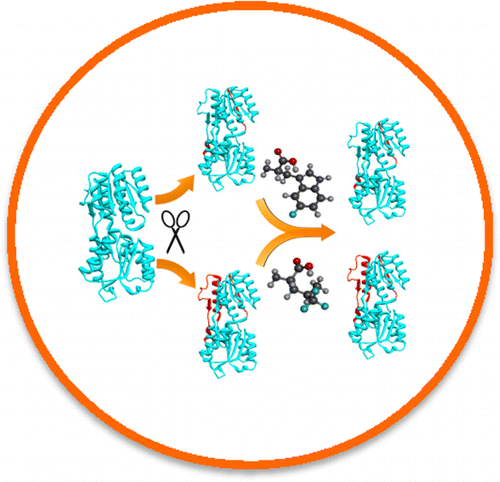
They turned to a protein that has already been explored as a good candidate for use in a continuous glucose monitoring system. It's a glucose/galactose binding protein (GBP) that changes shape when it attaches to glucose. They engineered it so it would be stable in and out of the body for long periods and so that it could also detect levels of glucose within the range that would be present in a person with diabetes.
More information: Glucose Recognition Proteins for Glucose Sensing at Physiological Concentrations and Temperatures, pubs.acs.org/doi/abs/10.1021/cb500132g
Journal information: ACS Chemical Biology
Provided by American Chemical Society