Researchers solve crystal structure of key biofilm protein
(Phys.org)—Researchers at the University of Cincinnati (UC) report that they have solved the crystal structure of a protein involved in holding bacterial cells together in a biofilm, a major development in their exploration of the causes of hospital-acquired infections.
The finding, the researchers say, enables them to have an atomic-level view of what the protein looks like and how it becomes "sticky" in the presence of zinc ions, forming an extensive adhesive contact crucial to the formation of infection-causing biofilms.
The researchers report their findings in the online Early Edition of PNAS, the official journal of the National Academy of Sciences. Andrew Herr, PhD, an associate professor in the department of molecular genetics, biochemistry and microbiology at UC and Ohio Eminent Scholar in structural biology, led the research and wrote the paper.
The research team, in addition to Herr, consisted of Deborah Conrady, PhD, now a postdoctoral fellow at the University of British Columbia, and Jeffrey Wilson, PhD, a former postdoctoral fellow at UC.
"Understanding the mechanisms of biofilm formation will allow us to combat the significant pathogenic advantages of biofilm-based infectious diseases," says Herr.
Hospital-acquired infections affect about 1.7 million people per year in the United States and result in an estimated 99,000 deaths annually, according to the Centers for Disease Control and Prevention. About two-thirds of all hospital-acquired infections can be traced to two staphylococcal species, Staphylococcus aureus—including methicillin-resistant strains (MRSA) that are particularly difficult to treat—and Staphylococcus epidermidis.
Staphylococci can grow as biofilms, which are specialized communities of bacteria that are highly resistant to antibiotics and immune responses. They are remarkably adhesive and can grow on many surfaces, including implanted medical devices such as pacemakers, heart valve replacements and artificial joints. Preventing or inhibiting the growth of such biofilms would dramatically reduce the incidence of staph infections.
Previously, researchers in Herr's lab had detailed findings that the presence of zinc is crucial to the formation of infection-causing biofilms. Zinc, they found, causes a protein on the bacterial surface to act like molecular Velcro, allowing the bacterial cells in the biofilm to stick to one another. Zinc chelation, a way to make the zinc unavailable to the bacteria, prevented biofilm formation by Staphylococcus epidermidis and Staphylococcus aureus.
In the new research, the investigators determined the atomic structure of a portion of an adhesive protein Aap bound to zinc by growing crystals of the protein, freezing them in liquid nitrogen and bombarding them with highly intense X-rays. They then measured how the X-rays were scattered by the crystal, and used those measurements to determine the 3D position of the atoms in the protein.
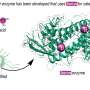
The protein, the researchers found, adopts an elongated flexible fold with zinc ions bridging two protein chains. The mode of assembly indicates that Aap is likely to form twisted rope-like structures between bacterial cells.
"We can see literally what the structure of the protein is," Herr says. "In other words, how it is put together, how it folds back on itself to form its unique shape and how two copies of the protein latch onto the zinc ion and stick together like molecular Velcro."
Knowing the structure allows researchers to understand which parts of the protein to target therapeutically, Herr says, which could provide new approaches for disrupting the formation of biofilms. The most practical applications might involve coatings for implanted medical devices, or rinses that a surgeon could use to clear the area around an implant.
The research project was supported by the National Institutes of Health and by a pilot grant from UC's Midwest Center for Emerging Infectious Diseases; Herr also had access to funds from the State of Ohio Eminent Scholars Program. The authors report no conflicts of interest.
Journal information: Proceedings of the National Academy of Sciences
Provided by University of Cincinnati