New substance may allow successful transplantation of 'marginal' livers
New research raises the possibility that the critically short supply of livers for organ donation could be expanded by treating so-called "marginal" livers with a substance that protects them from damage after being connected to recipients' blood supplies. The report appears in ACS' journal Molecular Pharmaceutics.
Ram Mahato and colleagues note that the need for liver transplants has grown over the years, though the number of available livers has not. Currently, more than 16,000 people are waiting for a liver in the U.S., but less than 7,000 liver transplants were performed during the entire year of 2010. This shortage has led organ transplant teams to consider using marginal, or damaged, livers, such as those with cholestasis — a build-up of bile. But transplanting a damaged liver has risks, including a higher risk that the organ will fail. To overcome this challenge, the researchers utilized a hedgehog-signaling inhibitor to increase the odds of a successful liver transplant.
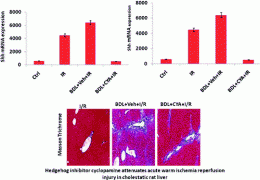
They found that a compound called cyclopamine prevented further injury to cholestatic livers after the blood supply was cut off then returned — a situation similar to what transplanted livers undergo. The research was performed in rats, which are stand-ins for humans in the laboratory. It provided "convincing evidence" that cyclopamine may protect cholestatic livers from additional damage after a transplant procedure and improve clinical outcomes for the patients.
More information: “Cyclopamine attenuates acute warm ischemia reperfusion injury in cholestatic rat liver: Hope for marginal livers”, Mol. Pharmaceutics, Article ASAP DOI: 10.1021/mp200115v
Abstract
Cholestasis is a significant risk factor for immediate hepatic failure due to ischemia reperfusion (I/R) injury in patients undergoing liver surgery or transplantation. We recently demonstrated that inhibition of Hedgehog (Hh) signaling with cyclopamine (CYA) before I/R prevents liver injury. In this study we hypothesized that Hh signaling may modulate I/R injury in cholestatic rat liver. Cholestasis was induced by bile duct ligation (BDL). Seven days after BDL, rats were exposed to either CYA or vehicle for 7 days daily before being subjected to 30 min of ischemia and 4 h of reperfusion. Expression of Hh ligands (Sonic Hedgehog, Patched-1 and Glioblastoma-1), assessment of liver injury, neutrophil infiltration, cytokines, lipid peroxidation, cell proliferation and apoptosis were determined. Significant upregulation of Hh ligands was seen in vehicle treated BDL rats. I/R injury superimposed on these animals resulted in markedly elevated serum alanine transaminase (ALT), aspartate transaminase (AST), total bilirubin accompanied with increased neutrophil recruitment and lipid peroxidation. Preconditioning with CYA reduced the histological damage and serum liver injury markers. CYA also reduced neutrophil infiltration, proinflammatory cytokines such as TNF-α and IL-1β expression of α-smooth muscle actin and type 1 collagen resulting in reduced fibrosis. Furthermore CYA treated animals showed reduced cholangiocyte proliferation, and apoptosis. Hepatoprotection by CYA was conferred by reduced activation of protein kinase B (Akt) and extracellular signal regulated kinase (ERK). Endogenous Hh signaling in cholestasis exacerbates inflammatory injury during liver I/R. Blockade of Hh pathway represents a clinically relevant novel approach to limit I/R injury in cholestatic marginal liver.
Provided by American Chemical Society