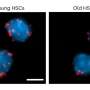
Immune cells regulate blood stem cells
Researchers in Bern, Germany, have discovered that, during a viral infection, immune cells control the blood stem cells in the bone marrow and therefore also the body's own defences. The findings could allow for new forms of therapy, such as for bone marrow diseases like leukaemia.
During a viral infection, the body needs various defence mechanisms – amongst other things, a large number of white blood cells (leukocytes) must be produced in the bone marrow within a short period of time. In the bone marrow, stem cells are responsible for this task: the blood stem cells. In addition to white blood cells, blood stem cells also produce red blood cells and platelets.
The blood stem cells are located in specialized niches in the bone marrow and are surrounded by specialized niche cells. During an infection, the blood stem cells must complete two tasks: they must first recognise that more blood cells have to be produced and, secondly, they must recognise what kind of.
Now, for the first time, researchers at the Department of Medical Oncology at the University of Bern and Bern University Hospital headed by Prof. Adrian Ochsenbein have investigated how the blood stem cells in the bone marrow are regulated by the immune system's so-called T killer cells during a viral infection. As this regulation mechanism mediated by the immune system also plays an important role in other diseases such as leukaemia, these findings could lead to novel therapeutic approaches. The study is being published in the peer-reviewed journal Cell Stem Cell today.
T Killer cells trigger defences
One function of T killer cells is to "patrol" in the blood and remove pathogen-infected cells. However, they also interact with the blood stem cells in the bone marrow. The oncologists in Bern were able to show that messenger substances secreted by the T killer cells modulate the niche cells. In turn, the niche cells control the production and also the differentiation of the blood stem cells.
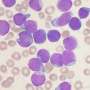
This mechanism is important in order to fight pathogens such as viruses or bacteria. However, various forms of the bone marrow disease leukaemia are caused by a malignant transformation of exactly these blood stem cells. This leads to the formation of so-called leukaemia stem cells. In both cases, the mechanisms are similar: the "good" mechanism regulates healthy blood stem cells during an infection, whilst the "bad" one leads to the multiplication of leukaemia stem cells. This in turn leads to a progression of the leukaemia.
This similarity has already been investigated in a previous project by the same group of researchers. "We hope that this will enable us to better understand and fight infectious diseases as well as bone marrow diseases such as leukaemia," says Carsten Riether from the Department of Clinical Research at the University of Bern and the Department of Medical Oncology at Bern University Hospital and the University of Bern.
More information: Christian M. Schürch, Carsten Riether, Adrian F. Ochsenbein: "Cytotoxic CD8+ T cells stimulate hematopoietic progenitors by promoting cytokine release from bone marrow mesenchymal stromal cells," Cell Stem Cell, 20 February 2014, in press. dx.doi.org/10.1016/j.stem.2014.01.002
Journal information: Cell Stem Cell
Provided by University of Bern