'Vicious cycle' shields, spreads cancer cells
A "vicious cycle" produces mucus that protects uterine and pancreatic cancer cells and promotes their proliferation, according to researchers at Rice University. The researchers offer hope for a therapeutic solution.
They found that protein receptors on the surface of cancer cells go into overdrive to stimulate the production of MUC1, a glycoprotein that forms mucin, aka mucus. It covers the exposed tips of the elongated epithelial cells that coat internal organs like lungs, stomachs and intestines to protect them from infection.
But when associated with cancer cells, these slippery agents do their jobs too well. They cover the cells completely, help them metastasize and protect them from attack by chemotherapy and the immune system.
Details of the new work led by biochemist Daniel Carson, dean of Rice's Wiess School of Natural Sciences, appear in the Journal of Cellular Biochemistry.
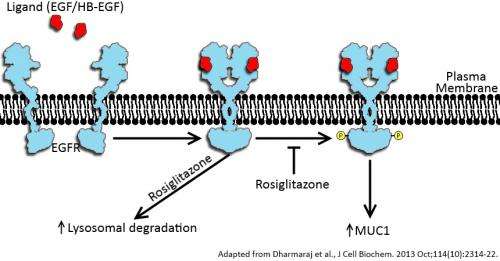
In the paper, Carson, lead author Neeraja Dharmaraj, a postdoctoral researcher, and graduate student Brian Engel described MUC1 overexpression as particularly insidious not only for the way it protects tumor cells and promotes metastasis, but also because the cells create a feedback loop in which epidermal growth factor receptors (EGFR) and MUC1 interact to promote each other.
Carson described EGFR as a powerful transmembrane protein that stimulates normal cell growth, proliferation and differentiation. "What hadn't been considered is whether this activated receptor might actually promote the expression of MUC1, which would then further elevate the levels of EGFR and create this vicious cycle.
"That's the question we asked, and the answer is 'yes,'" he said.
Carson compared mucus to Teflon. "Things don't stick to it easily, which is normally what you want. It's a primary barrier that keeps nasty stuff like pathogenic bacteria and viruses from getting into your cells," he said.
But cancer cells "subvert systems and find ways to get out of control," he said. "They auto-activate EGFR by making their own growth factor ligands, for example, or mutating the receptor so it doesn't require the ligand anymore. It's always on."
Mucin proteins can then cover entire surface of a cell. "That lets (the cell) detach and move away from the site of a primary tumor," while still preventing contact with immune system cells and cytotoxins that could otherwise kill cancer cells, Carson said.
Hope comes in the form of a controversial drug, rosiglitazone, in the thiazolidinedione class of medications used in diabetes treatment, he said. The drug is suspected of causing heart problems over long-term use by diabetes patients. But tests on cancer cell lines at Rice found that it effectively attenuates the activation of EGFR and reduces MUC1 expression. That could provide a way to weaken the mucus shield.
"Chronic use of rosiglitazone can produce heart problems in a subset of patients, but if you're dying of pancreatic cancer, you're not worried about the long term," Carson said. "If you can reduce mucin levels in just a few days by using these drugs, they might make cancer cells easier to kill by established methods."
He said more work is required to see if rosiglitazone or some variant is suitable for trials. "We think it's best to understand all the effects," he said. "That might give us a rational way to modify these compounds, to avoid unwanted side effects and focus on what we want them to do."
Carson is the Schlumberger Chair of Advanced Studies and Research and a professor of biochemistry and cell biology with a joint appointment in the Department of Biochemistry and Molecular Biology at the University of Texas MD Anderson Cancer Center. He also is Rice's vice provost for strategic partnerships.
More information: onlinelibrary.wiley.com/doi/10 … 2/jcb.24580/abstract
Journal information: Journal of Cellular Biochemistry
Provided by Rice University