This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
reputable news agency
proofread
What is CRISPR? What to know about the transformative gene-editing tool

Over the past 10 years, CRISPR has been transformative for research, enabling gene editing that is fast, simple and precise, experts say.
The first paper showing that CRISPR could be used to edit the genes of mammals was published 10 years ago this month. Since then, it has been used in research laboratories across the world and is being tested in treatments for cancer and rare diseases and for making crops that are heartier and more resistant to disease and climate change.
CRISPR gene editing is fast, simple and precise, researchers say.
"There are many instances that without CRISPR, our life as scientists would be much more difficult," said Beverly Davidson, a neuroscientist at The Children's Hospital of Philadelphia.
Gene editor Fyodor Urnov compared DNA sequencing—a detailed reading of the genome—to a powerful telescope. CRISPR, meanwhile, "allows us to fly to these newly discovered galaxies and do something useful once we're there," he said. "It gives us absolutely unprecedented insight into the functioning of every biological system from tiny yeast to the human being."
CRISPR has already been used to discover the biological basis of diseases that have then led to treatments, he said. "And that's within 10 years."
Here's what to know.
What is CRISPR used for?
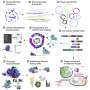
In nature, CRISPR, an acronym for "clustered regularly interspaced short palindromic repeats," serves as an immune system for bacteria. Scientists have repurposed it to make gene editing more precise and simpler to use.
CRISPR has the ability to find a specific spot in a strand of DNA and make a cut, add or swap a genetic "letter" or even a word.
Advanced forms of CRISPR allow researchers to rapidly screen diseased versus normal cells, finding targets for gene editing.
Scientists used to spend years and "tons of money" breeding mice that had the same genetic changes as people with rare inherited diseases, said Dr. Tippi MacKenzie, a pediatric and fetal surgeon at the University of California San Francisco. "Now you can do it in a matter of weeks."
Has CRISPR been used on humans?
In November 2018, Chinese scientist He Jiankui sparked a global scandal by admitting he had used the gene editing tool to edit embryos and create "CRISPR babies."
Most scientists and medical ethicists support the idea of using gene editing to improve the life of someone with a terrible disease. Such changes help address illness while the person is alive.
But mainstream scientists and companies are not working on so-called germline editing, though there may be some rogue actors still considering it.
"It doesn't even make sense" to do this, said Dr. John Leonard, president and CEO of Intellia Therapeutics, which is developing CRISPR-based treatments for rare diseases and cancer. Virtually all conditions that could benefit from germline editing can be treated or prevented another way, he said.
Since 2016, CRISPR has been used in clinical trials to treat patients with blood cancer. More recent research has tested CRISPR gene edits on people with rare diseases caused by single gene mutations.
"We're trying to create answers for people who actually have diseases," Leonard said.
What is CRISPR-Cas9?
In June 2012, biochemists Jennifer Doudna and Emmanuelle Charpentier published a paper describing how CRISPR works as a bacterial immune system. They revealed that Cas9, short for CRISPR-associated endonuclease 9, acts like a scissors, snipping DNA. The two women earned a Nobel Prize in chemistry in 2020 for their findings.
"The protein Cas9 to DNA is like the cursor of your mouse that you use to 'click' on a segment of text you want changed," said Urnov, of the University of California, Berkeley.
Delivered to the right spot with an RNA, Cas9 cuts both strands of a piece of DNA. When the strands are put together again, a few letters of genetic text are lost. Researchers use that ability get rid of a toxic gene.
In people with sickle cell disease, for instance, researchers are using Cas9 to make a genetic snip enabling a patient's body to once again make a substance called fetal hemaglobin. Fetal hemaglobin, typically turned off in the first year of life, reduces the sickling of red blood cells that causes patients' severe pain and organ damage.
Using CRISPR to treat sickle cell, Urnov said, is essentially like pulling a spare tire out of a trunk to replace a flat.
(c)2023 USA Today
Distributed by Tribune Content Agency, LLC.