How a harmless environmental bacterium became the dreaded hospital germ Acinetobacter baumannii
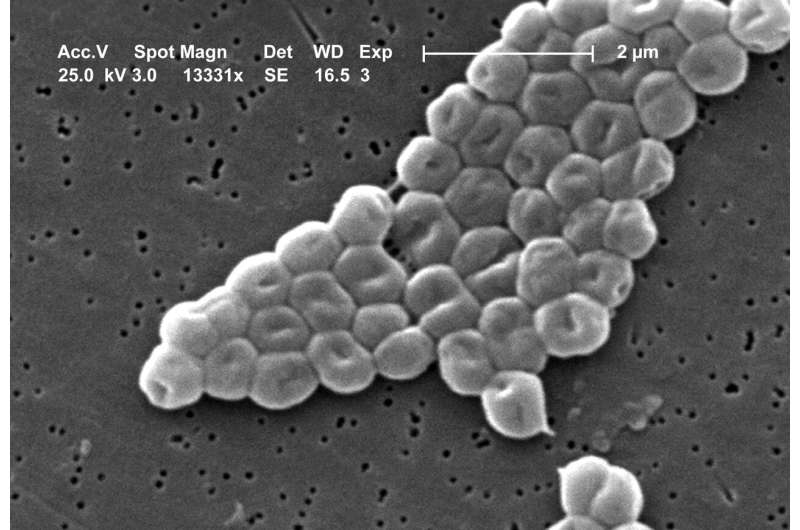
Each year, more than 670,000 people in Europe fall ill due to pathogenic bacteria that exhibit antibiotic resistance, and 33,000 die of the diseases they cause. Especially feared are pathogens that are resistant to several antibiotics at the same time. Among them is the bacterium Acinetobacter baumannii, which is today dreaded above all as a "hospital superbug." Up to five percent of all hospital-acquired bacterial infections are caused by this germ alone.
A. baumannii is right at the top of a list of candidates for which, according to the World Health Organization (WHO), new therapies must be developed. This is because the pathogen—due to a flexible genome—easily acquires new antibiotic resistance. At the same time, infections are not only occurring more and more outside the hospital environment but also leading to increasingly severe progression. However, a prerequisite for the development of new therapeutic approaches is that we understand which properties make A. baumannii and its human pathogenic relatives, grouped in what is known as the Acinetobacter calcoaceticus-baumannii (ACB) complex, a pathogen.
A team led by bioinformatician Professor Ingo Ebersberger from Goethe University Frankfurt/ LOEWE Centre for Translational Biodiversity Genomics (LOEWE-TBG) has now reached a milestone in this understanding. The team is composed of members of Research Unit 2251 of the German Research Foundation and other national and international partners, among them scientists of Washington University School of Medicine, St Louis, U.S.
For their analysis, the team made use of the fact that a large proportion of the members of the Acinetobacter genus are harmless environmental bacteria that live in water or on plants or animals. Thousands of complete genome sequences both of these as well as of pathogenic Acinetobacter strains are stored in publicly accessible databases.
By comparing these genomes, the researchers were able to systematically filter out differences between the pathogenic and the harmless bacteria. Because the incidence of individual genes was not particularly conclusive, Ebersberger and his colleagues concentrated on gene clusters, that is, groups of neighboring genes that have remained stable during evolution and might form a functional unit. "Of these evolutionarily stable gene clusters, we identified 150 that are present in pathogenic Acinetobacter strains and rare or absent in their non-pathogenic relatives," says Ebersberger, summing up. "It is highly probable that these gene clusters benefit the pathogens' survival in the human host."
Among the most important properties of pathogens is their ability to form protective biofilms and to efficiently absorb micronutrients such as iron and zinc. And indeed, the researchers discovered that the uptake systems in the ACB group were a reinforcement of the existing and evolutionary older uptake mechanism.
Particularly exciting is the fact that the pathogens have evidently tapped a special source of energy: they can break down the carbohydrate kynurenine produced by humans, which as a messenger substance regulates the innate immune system. The bacteria apparently kill two birds with one stone in this way. On the one hand, breaking down kynurenine supplies them with energy, and on the other hand, they could possibly use it to deregulate the host's immune response.
Ebersberger is convinced: "Our work is a milestone in understanding what's different about pathogenic Acinetobacter baumannii. Our data are of such a high resolution that we can even look at the situation in individual strains. This knowledge can now be used to develop specific therapies against which, with all probability, resistance does not yet exist."
Their study is published in PLOS Genetics.
More information: Bardya Djahanschiri et al, Evolutionarily stable gene clusters shed light on the common grounds of pathogenicity in the Acinetobacter calcoaceticus-baumannii complex, PLOS Genetics (2022). DOI: 10.1371/journal.pgen.1010020
Journal information: PLoS Genetics
Provided by Goethe University Frankfurt am Main