April 2, 2020 feature
Bioengineering biomimetic human small muscular pulmonary arteries
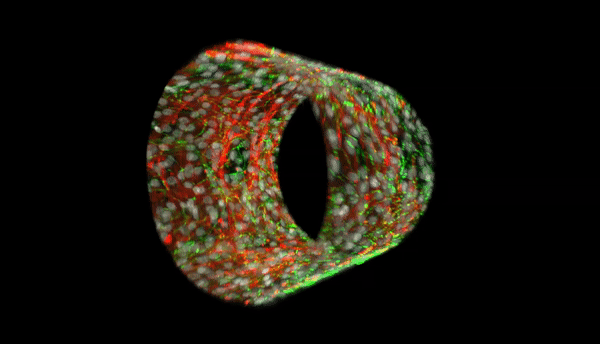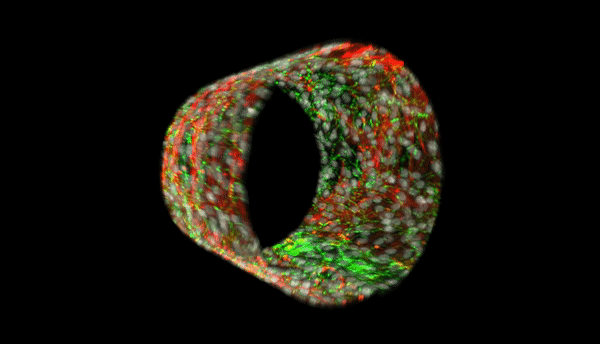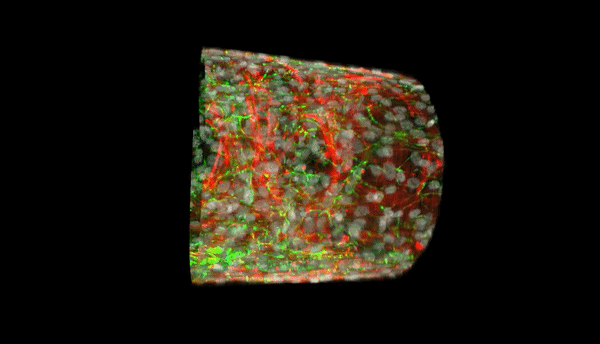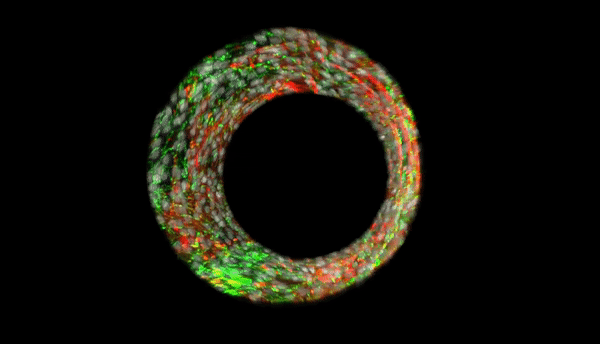
During the progression of pulmonary hypertension, structural and functional changes in the small muscular arteries play a significant role and contribute to the disease. Bioengineers aim to develop advanced, anatomically biomimetic in vitro models of microvessels, since non-human vessels are not an accurate representation of the human microvascular architecture and microenvironment. In a new report now on Science Advances, Qianru Jin and a multidisciplinary research team at the Johns Hopkins University, U.S., described a new method for parallel biofabrication of a photopatterned, self-rolled and biomimetic pulmonary arterial microvessel of adjustable size and architecture.
The microvessel features were anatomically accurate with layering and patterning of aligned human smooth muscle cells, extracellular matrix and endothelial cells. The structures exhibited notably increased longevity in endothelial cells and produced nitric oxide . The scientists used computational image processing to obtain high-resolution 2-D simulations of cells and proteins, the new work provides a complete model to bioengineer multicellular tissues based on precise three-dimensional (3-D) spatial positioning. The new biomimetic platform will allow medical researchers to investigate microvascular pathobiology in human disease.
In major cardiovascular disease (CVD) including pulmonary heart disease, the dysregulation of vasomotor tone in arterial vessels can increase peripheral resistance. Researchers use the term human "small muscular pulmonary arteries" (hSMPA) to describe the microvasculature resistance vessels in the supply-side during human pulmonary circulation. Such vessels are equivalent to arteries during systemic circulation. While existing in-lab models do not adequately summarize the complexity of the vasculature, animal models of CVD are also limited since they deviate from the human vascular infrastructure. Microvascular tissue-inspired in vitro models will provide improved efficiency during basic and translational research to advance CVD pathophysiology. For example, tissue engineers had previously developed tissue-on-a-chip or organ-on-a-chip systems to combine cell culture with microfluidics to mimic physiological environments and provide cues to investigate pathophysiology and drug discovery or development. However, the microfabricated fluidic chips cannot recapitulate the native morphology of microvessels and require special machinery for scaled-up production. To address these existing limits, Jin et al. created biomimetic constructs with essential features of hSMPAs (human small muscular pulmonary arteries).
To achieve anatomically correct layering, the scientists focused on vascular smooth muscle cell (VSMC) alignment and growth patterns as key features during pulmonary hypertension pathogenesis. The approach to engineer the accurate cytoarchitecture for hSMPAs ensured accurate biomimicry of the model to test and recapitulate disease pathophysiology. The team used photolithography and biocompatible thin film deposition to precisely pattern human cells and recapitulate the microarchitecture of the vessel wall.
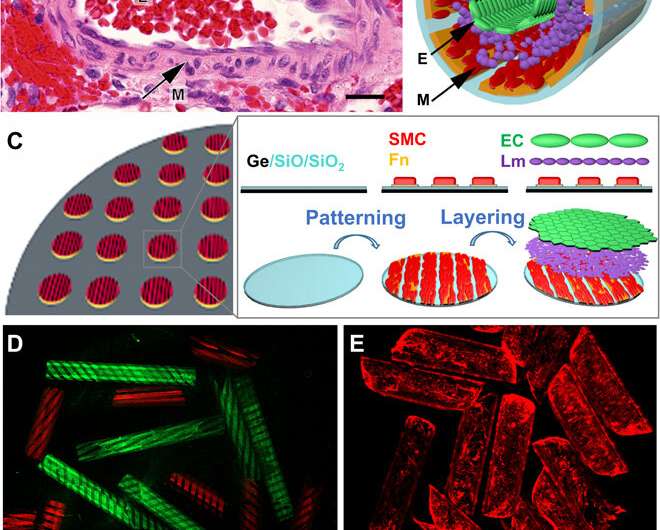
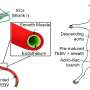
Bioengineering the biomimetic human small muscular pulmonary artery (hSMPA)
The research team combined the key features of hSMPAs including their diameters ranging from 50 to 300 µm, a confluent intimal lining of endothelial cells (EC) and an aligned VSMC (vascular smooth muscle cell) population. They then engineered a silicon monoxide/silicon dioxide (SiO/SiO2) bilayer, self-folding film at the wafer scale and incorporated photolithography, physical vapor deposition and protein patterning during the work. The silicon dioxide was amenable to surface modification, allowing them to pattern matrix proteins on the luminal surface of the tubular constructs. Jin et al. used Germanium (Ge) beneath the SiO/SiO2 bilayer as a cell-friendly construct to prevent the need for harsh chemicals during assembly of the pulmonary artery. The surface provided tunable detachment to optimize the adhesion of constituent cell layers and achieved uniform cell coverage during the experiments.
Mechanical considerations for tubular constructs and characterizing cell coverage
The team then developed a mechanical model and included the elastic modulus (ratio of stress and strain), substrate thickness and radius of curvature to study the stiffness of vascular wall cells exposed to the tubular constructs. The elastic moduli of SiO and SiO2 exceeded that of the native pulmonary arterial vessel wall by six orders of magnitude. To model the flexural stiffness that cells are exposed to in their native environment, Jin et al. then considered a theoretical model. Using finite element analysis, they verified the theoretical scaling law and tested the proportionality constant representing cellular traction. Based on scaling analysis, the SiO/SiO2 tubular constructs approximated the micromechanics of the hSMPA wall, while the flexural stiffness of the biodegradable constructs eventually resembled the native state, enabling enhanced biocompatibility of the materials.
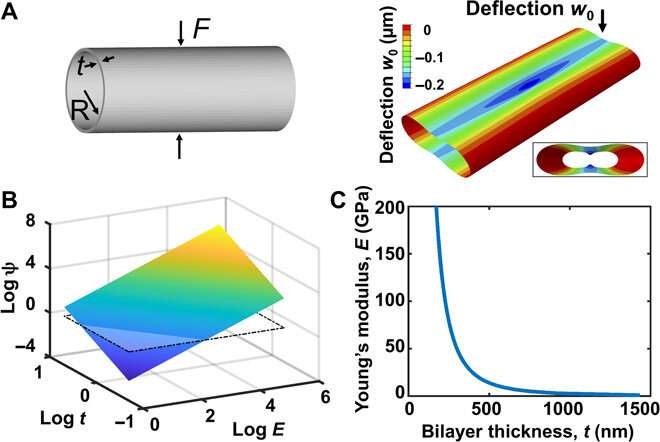
After 48 hours of seeding human pulmonary microvascular endothelial cells (HPMECs) on the constructs, they observed a confluent monolayer of cells on the luminal surface of the biomimetic microvessel. They were unable to image the entire 3-D biomimetic microvessel due to the depth and curvature of the structure, which they addressed using a refractive-index matched mountant. Thereafter they obtained sequential imaging of each side of the sample to obtain a z-stack of the entire tube for 3-D viewing.
Coculturing HPMECs and the human pulmonary artery smooth muscle cells (HPASMCs).
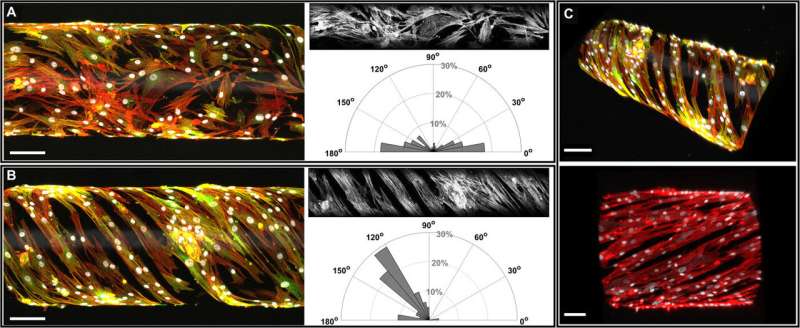
To mimic the structure and composition of human small muscular pulmonary arteries, the team seeded human pulmonary artery smooth muscle cells (HPASMCs) on top of the material bilayer and then deposited laminin – a major component of the inner elastic lamina. They observed distinct and anatomically correct layering of the two cell types at high resolution in 3-D. Vascular smooth muscle cells (VSMCs) in the medial layer of human small muscular pulmonary arteries (hSMPA) are typically arranged circumferentially to effect pulmonary microvascular flow and vasoreactivity. However, computational models are unable to capture this alignment or allow tunability to effectively address the importance of VSMCs in the hSMPA cytoarchitecture or their contributions to pulmonary vascular resistance. Jin et al. therefore used lithography and patterned fibronectin on the films before releasing and rolling the biomimetic microvessels. The work allowed them to observe the integrity of the pattern to be preserved. When the scientists cultured HPASMCs on these surfaces, the cells demonstrated high fidelity and anatomically accurate cell alignment. The team will therefore introduce controlled directionality of patterning by adding boundary conditions through such mask designs in the future.
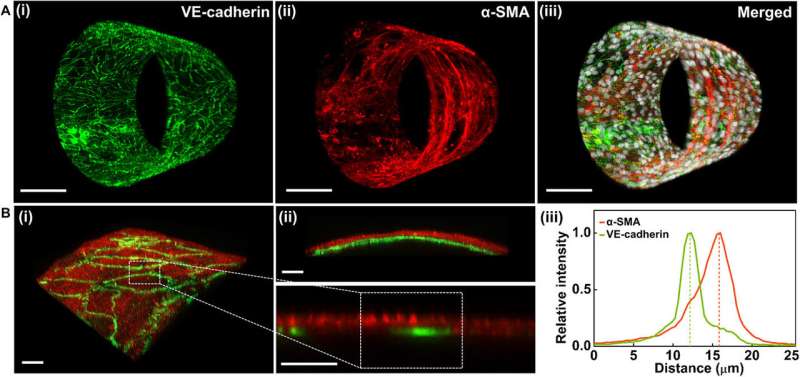
Improved cellular longevity and signaling in biomimetic pulmonary arteries
Since long-term cell viability is important in tissue engineering, the research team observed both endothelial cells (HPMECs) and smooth muscle cells (HPASMCs) cocultured in the biomimetic pulmonary arteries (hSMPA) to demonstrate substantial longevity. The HPMECs also showed substantial nitric oxide production within biomimetic vessels, which increased four-fold in 48 hours compared to control cells cultured on flat films of SiO/SiO2. The data showed how biomimetic pulmonary arteries enhanced robust function of vascular wall cells.
In this way, Qianru Jin and colleagues developed mass-producible, self-folding tunable constructs that allowed precise, multicellular layering for enhanced viability and functionality of human pulmonary vascular cells in the lab. The team described the first integrated approach to pattern, generate, image and analyze microaligned and layered cellular and tissue-level functions within biomimetic in vitro pulmonary arteries. The work provides an important step to form an in vitro platform and study vascular wall biology in an anatomically accurate human tissue-specific environment. The scientists expect the new approach to provide insights to understand cardiovascular disease and other pressing microvascular-based public health challenges.
More information: Qianru Jin et al. Biomimetic human small muscular pulmonary arteries, Science Advances (2020). DOI: 10.1126/sciadv.aaz2598
D. Huh et al. Reconstituting Organ-Level Lung Functions on a Chip, Science (2010). DOI: 10.1126/science.1188302
Vikram Gurtu et al. A Paradigm Shift Is Needed in the Field of Pulmonary Arterial Hypertension for Its Entrance Into the Precision Medicine Era, Circulation Research (2016). DOI: 10.1161/CIRCRESAHA.116.309689
Journal information: Science Advances , Science , Circulation Research
© 2020 Science X Network