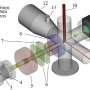
Finger-mounted optical probe designed to improve breast cancer removal

Researchers have developed the first wearable probe that enhances the sense of touch by imaging and quantifying the stiffness and elasticity of biological tissue. The device is being developed to improve the surgical removal of breast cancer and might also be useful for brain and liver surgery and other types of cancer.
In The Optical Society (OSA) journal Biomedical Optics Express, researchers from the University of Western Australia (UWA) describe the new device, which incorporates a fiber probe into a wearable thimble.
During breast conserving surgery, the most common surgical treatment for breast cancer, surgeons touch and compress tissue to confirm that the stiffer cancerous tissue was removed. Histopathological testing is then performed days later to ensure that the whole tumor was removed. Today, 20 to 30 percent of patients undergoing this type of surgery require another procedure because the histopathological tests show that cancerous cells remain.
"Our new probe aims to enhance the surgeon's subjective sense of touch through quantified, high-resolution imaging of tissue stiffness," said Rowan W. Sanderson, first author of the paper. "This could make it easier to detect and remove all the cancerous tissue during the first breast conserving surgery, which would reduce the physical and psychological burden and cost that accompanies re-excision."
Turning touch into images
The finger-mounted probe uses a technique called quantitative micro-elastography (QME) to translate the sense of touch into high-resolution images. QME uses measurements from an optical imaging technique called optical coherence tomography (OCT), which generates high-resolution, depth-resolved images of tissue structure by measuring the reflections, or 'echoes,' of light.
To use the device, the finger-mounted probe is pressed perpendicularly into the tissue while OCT images are recorded. "By preserving the sense of touch, we aim to conserve the existing clinical workflow and increase the likelihood that this technology would be adopted for wider clinical use," said Sanderson.
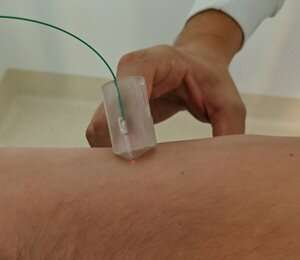
For accurate elasticity measurements, the researchers developed new signal processing methods with custom algorithms to deal with inconsistent motion and pressure during scanning. 3-D printing helped them quickly produce prototypes of the probe's outer casing in a simple and cost-effective manner.
"Our finger-mounted probe can accurately detect microscale changes in stiffness, which are indicative of disease," said Sanderson. "The small size makes it ideal for imaging in confined spaces such as a surgical cavity."
Tissue tests
To validate the probe, they began by testing it on materials, known as silicone phantoms, designed to mimic healthy and diseased tissues in the breast. These tests showed that the finger-mounted probe had an accuracy of 87 percent, which was slightly lower than a conventional benchtop QME system, but still sufficiently high for potential clinical use.
They then used the probe to measure the change in stiffness caused by heating a sample of kangaroo muscle. This experiment showed the muscle sample underwent a 6-fold increase in stiffness following the heating process. A preliminary 2-D image was obtained by scanning the probe laterally across a silicone phantom containing a stiff inclusion. Although it showed lower accuracy than the experiment performed without scanning, the researchers say that the prospect for imaging by swiping the operator's finger is very encouraging. "The contrast between sample features was still evident, which indicates that 2-D scanning holds a lot of promise going forward," said Sanderson.
The researchers are now working to embed the optical components of the probe into a surgical glove that would preserve the touch sensitivity and dexterity of manual palpation. They are also improving the accuracy of the 2-D scanning.
This work forms part of a broader project to develop novel tools to improve surgery. The research team has also developed both bench-top and handheld implementations of micro-elastography. In addition to efforts within the University, the team also works closely with OncoRes Medical, a UWA start-up company formed in late 2016 to commercialize the micro-elastography technology.
More information: Rowan W. Sanderson et al. Finger-mounted quantitative micro-elastography, Biomedical Optics Express (2019). DOI: 10.1364/BOE.10.001760
Journal information: Biomedical Optics Express
Provided by Optical Society of America