Scientists find old antibiotic may selectively kill dangerous skin cancer cells
An old antibiotic, called nifuroxazide, could selectively kill dangerous cells within melanomas, the deadliest type of skin cancer, scientists from the Medical Research Council (MRC) Institute of Genetics and Molecular Medicine at the University of Edinburgh have found.
The study, published in the journal Cell Chemical Biology, found the drug showed promise for complementing existing melanoma therapies. The drug's effect on melanoma cells was tested in mice and samples from human tumours and the scientists caution more research is needed to determine if it will be effective in people.
Within a single tumour there can be variation in the properties of the cells, with some more dangerous than others, in terms of their potential to support growth or become resistant to drug treatment. Many of the more dangerous cells in melanoma tumours produce a lot of an enzyme called aldehyde dehydrogenase 1 (ALDH1).
Current research into therapies has focused on blocking ALDH1, but in this study the researchers went a step further and aimed to selectively kill cells producing high ALDH1.
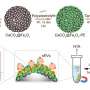
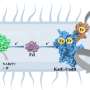
They used the drug nifuroxazide, an antibiotic, that is activated by the enzyme ALDH1, which means that it only becomes toxic once it is inside cells producing ALDH1.
Using samples of human melanomas implanted in mice the researchers showed that the nifuroxazide therapy killed the tumour cells that produced a lot of ALDH1, without significant toxicity to other cells in the body.
The researchers hope that the strategy may complement existing melanoma treatments, called BRAF and MEK inhibitors. Currently, some people's tumours develop resistance to BRAF and MEK inhibitors and the researchers found that some of these resistant tumours were high in ALDH1.
In the lab, the researchers simulated this by treating cancer cells lines with BRAF and MEK inhibitors, which increased the number of cells with high levels of ALDH1 and made the cells especially sensitive to nifuroxazide treatment.
Dr. Liz Patton from the MRC Institute for Genetics and Molecular Medicine at the University of Edinburgh, who led the research, said: "There won't be one magic bullet for targeting melanoma—the variations that exist within the cancers mean there will need to be combination therapies. When people are given BRAF or MEK drugs to treat melanoma it can result in the tumours having more cells with high levels of ALDH, so we think that's a really important target. We've shown this antibiotic that's used mostly to target intestinal bacteria can also target and kill cancer cells high in the enzyme ALDH1."
"It's great that this antibiotic is approved for use in humans, but it wasn't designed as a cancer drug, so we still need to find out if it's safe and effective for cancer in humans—for example, can it get to the cancer in the body and are the doses needed safe? We may need to take the concept for how this antibiotic works and re-design it to make it better at killing cancer."
Dr. Nathan Richardson, head of molecular and cellular medicine at the MRC, said: "This imaginative study exploits the sensitivity of some cancer cells to an existing antibiotic and could reveal an exciting new approach to both combination treatment and 'personalised' medicine by directly targeting drug resistance—a key priority for the MRC."
'ALDH1 bio-activates nifuroxazide to eradicate ALDH(High) melanoma-initiating cells' by Sarvi et al is published in Cell Chemical Biology.
More information: Cell Chemical Biology (2018). DOI: 10.1016/j.chembiol.2018.09.005
Journal information: Cell Chemical Biology
Provided by Medical Research Council