Watching gene-editing at work to develop precision therapies
University of Wisconsin-Madison engineers have developed methods to observe genome editing in action—and they're putting those capabilities to work to improve genetic engineering techniques. With support from a five-year, $1.8 million award from the National Institutes of Health, the new project could pave the way toward personalized treatment for genetic diseases.
"Ultimately, the knowledge we gain from this project has the potential to set the foundation for new preclinical platforms in precision medicine," says Krishanu Saha, an assistant professor of biomedical engineering at UW-Madison and the principal investigator on the project.
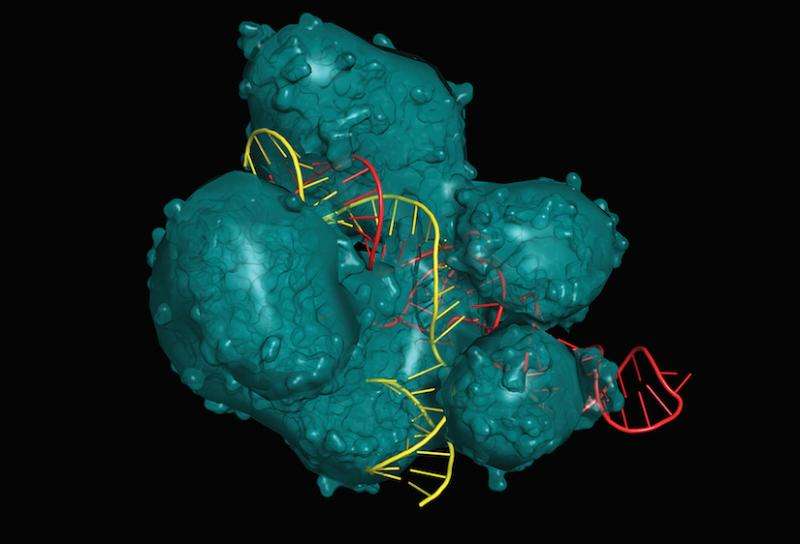
In recent years, researchers have learned how to use a tool called CRISPR-Cas9 to create specific changes within the molecules that make up life's instruction manual – the DNA double helices inside of all of the individual cells of every living thing on the planet.
"CRISPR-Cas9 lets researchers rewrite the genome in a very precise manner," says Saha.
Editing genomes offers the potential to correct the problems underlying previously incurable conditions—such as the debilitating blood disease sickle-cell anemia, the fatal lung disorder cystic fibrosis, or the blindness-causing Leber's congenital amaurosis. Because these diseases arise due to well known mishaps in the DNA, the ability to alter genomes with CRISPR-Cas9 could someday make such serious conditions a thing of the past.
But CRISPR-Cas9 is not a perfect editor. Sometimes the tool doesn't function very efficiently; other times, it makes changes in unexpected places. Researchers have tried to improve CRISPR-Cas9 by making structural tweaks to some of the components, but it is still unclear why some work better than others. These obstacles currently prevent most therapies from being safe to use in patients.

One of the main hurdles between CRISPR-Cas9 and the clinic is that much of what actually happens inside cells while the tool makes its edits has been mysterious.
"There's been a gap in understanding how several components of CRISPR-Cas9 achieve gene modification in human cells," says Saha. "Until we understand why some strategies fail and why some succeed, the use of genome surgery tools will be limited."
Saha's lab developed one method to help solve that mystery. The researchers found a way to label both different parts of cells and CRISPR-Cas9 in such a manner that they may observe important changes that occur while genome-editing happens in real-time.
The researchers will use those techniques to monitor CRISPR-Cas9 as it works inside cells in Petri dishes that mimic tissues from real patients. They will draw on their expertise working with stem cells to make miniature model organs in which to test different genome-editing strategies.
"This project is different from the status quo," says Saha. "Systematically changing multiple components of CRISPR-Cas9 at a time to test in patient-derived cells will lead to greater understanding of the biological processes important for genome surgery."
Over the next five years, the researchers will investigate multiple approaches to correcting the problems for several genetic diseases in numerous different types of tissues. The work is supported by a relatively new type of grant from the NIH, called the Maximizing Investigators Research Award (MIRA). The MIRA program aims to boost scientific productivity and innovation by providing both greater stability in funding, and more freedom to pursue revolutionary research. Saha is one of 93 promising young investigators nationwide identified for the transformative potential of his work.
Provided by University of Wisconsin-Madison