Antigen-specific targeting of immune system offers treatment approach to improve efficacy of biologic drugs
Selecta Biosciences, Inc., a clinical-stage biopharmaceutical company developing targeted antigen-specific immune therapies for rare and serious diseases, announced today that Nature Nanotechnology has published an article that presents preclinical results from Selecta's research which demonstrate the broad potential applicability of Selecta's novel immune tolerance platform. Details that elucidate the mechanism of action of the company's immune tolerance therapy, SVP-Rapamycin (SEL-110), were also shown. Data in the publication support the Company's lead clinical program, showing Selecta's SVP-Rapamycin (SEL-110) induces antigen-specific immune tolerance and mitigates the formation of anti-drug antibodies (ADAs) to biologic drugs, including pegsiticase (for gout) and adalimumab (for rheumatoid arthritis).
"Undesired immune responses affect both the efficacy and safety of marketed biologic therapies and the development of otherwise promising new technologies. Selecta's SVP platform positions the company to enhance biologic therapy and to advance a pipeline of proprietary products that meet the therapeutic needs of patients with rare and serious diseases," said Werner Cautreels, PhD,Chairman of the Board, CEO and President of Selecta Biosciences. "This publication in Nature Nanotechnology highlights the mechanism by which Selecta's proprietary nanoparticles induce lasting antigen-specific tolerance. We believe that SVP-Rapamycin has the potential to mitigate ADAs against a broad range of biologic therapies."
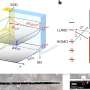
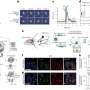
In the Nature Nanotechnology journal article, Selecta presents validation of the immune tolerance mechanism of action of the company's technology, demonstrating that poly(lactic-co-glycolic acid) (PLGA) nanoparticles encapsulating rapamycin, but not free rapamycin, are capable of inducing durable immunological tolerance to co-administered proteins. This robust immune tolerance is characterized immunologically by: (1) induction of tolerogenic dendritic cells; (2) an increase in regulatory T cells; (3) reduction in B cell activation and germinal center formation; and (4) inhibition of antigen-specific hypersensitivity reactions.
Data presented in the journal article support the Company's clinical lead program in gout, showing that intravenous co-administration of tolerogenic nanoparticles with pegylated uricase inhibited the formation of ADAs in mice and nonhuman primates and normalized serum uric acid levels in uricase-deficient mice. Underscoring the broad potential of the approach, results additionally show that subcutaneous co-administration of nanoparticles with adalimumab durably inhibited ADAs, resulting in normalized pharmacokinetics of the anti-TNFα antibody and protection against arthritis in TNFα transgenic mice.
In the published research, the induction of specific immune tolerance by SVP-Rapamycin (SEL-110) versus chronic immune suppression is supported by the findings that: (1) antigen must be co-administered at the time of SVP-Rapamycin (SEL-110) treatment; (2) immune tolerance is durable to many challenges of antigen alone; (3) animals tolerized to a specific antigen are capable of responding to an unrelated antigen, meaning that SVP-Rapamycin (SEL-110) does not induce a broad immune suppression; and (4) activation of naïve T cells is inhibited when adoptively transferred into previously tolerized mice. In contrast, daily administration of free rapamycin, at five times the total weekly rapamycin dose as that administered in the SVP-Rapamycin, was observed to transiently suppress the immune response, but did not induce durable immunological tolerance.
More information: Improving the Efficacy and Safety of Biologic Drugs with Tolerogenic Nanoparticles, Nature Nanotechnology, nature.com/articles/doi:10.1038/nnano.2016.135
Journal information: Nature Nanotechnology
Provided by Selecta Biosciences