Study reveals workings of mysterious 'relief valve' that protects cells from swelling

A team led by scientists at The Scripps Research Institute (TSRI) has solved a long-standing mystery in cell biology by showing essentially how a key "relief-valve" in cells does its job.
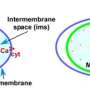
The relief valve, known as VRAC (volume-regulated anion channel), normally keeps cells from taking in too much water and swelling excessively. But VRAC's importance to cellular health is just beginning to be understood—already it has been tentatively linked to stroke-induced brain damage, diabetes, immune deficiency and even cancer treatment resistance.
In a study published in Cell on January 28, 2016, the scientists showed that VRAC is a complex structure with five different protein subunits—the precise mix of which determines its relief-valve properties. The team also determined that VRAC's relief-valve function is activated not by the physical swelling of a cell per se, but by a closely linked event: the low concentration of dissolved ions that results from a sudden flow of water into a cell.
"Knowing how VRAC is assembled and how it works is important not only because it is a fundamental regulatory mechanism in cells, but also because it seems to have relevance for a variety of diseases and conditions," said principal investigator Ardem Patapoutian, a professor at TSRI and a Howard Hughes Medical Institute (HHMI) Investigator.
Sorting Through the Molecular Soup
Scientists discovered VRAC's existence decades ago, but only recently began to identify its components. In early 2014, Patapoutian's laboratory and a separate group in Germany discovered independently that one VRAC subunit is a protein called LRRC8A (SWELL1), which is necessary for VRAC to function properly. It was apparent at the time, however, that VRAC has other subunits.
In the new study, Patapoutian and his team sought a more complete understanding of how VRAC is put together and how it senses volume changes.
Knowing that LRRC8A is always present in VRAC, co-first author Zhaozhu Qiu, a postdoctoral fellow in the Patapoutian lab and at the Genomics Institute of the Novartis Research Foundation (GNF), created test cells that produce LRRC8A with a special protein tag attached. The tagged LRRC8A were used as a handle to pull the full VRAC complex out of the molecular soup contained in cells.
Co-first author Ruhma Syeda, also a postdoctoral fellow in the Patapoutian lab, led the effort to put purified VRAC complexes into model cell membranes (lipid bilayers) to measure the conductance of charged ions. The results were startling. Although an ion channel typically has a sharply defined single channel conductance, measurements of VRAC suggested a broad range of conductances.
Prior research had suggested that the VRAC structure can include other members of the LRRC8 family besides LRRC8A, namely LRRC8B, LRRC8C, LRRC8D and/or LRRC8E. Qiu and Stuart Cahalan, another postdoctoral fellow, therefore created a set of cell lines in which genes for one or more of the LRRC8 proteins were deleted. With this and other methods, the team established that VRAC is in fact a diverse family of ion channels, each of which has approximately six protein subunits. At least one subunit of any VRAC structure is LRRC8A, but the other subunits appear to be a variable mix of LRRC8B-E proteins. That variability of composition leads to different charge-flow properties when channel complexes were measured in the minimalistic bilayer system. Swetha Murthy, a postdoctoral fellow, and Adrienne Dubin, an assistant professor of neuroscience (and co-corresponding author), determined that charge-flow properties of single VRAC channels on intact swollen cells were also dictated by the subunit combination.
"We speculate that different cell types need different forms of VRAC to cope with their different environments—that's an idea we're keen to test," said Qiu.
"This finding also suggests that subtle variations in VRAC's composition can have profound effects on how it works in cells and potentially contributes to disease," said Patapoutian.
How to Sense a Swelling Cell
Perhaps the biggest unanswered question about VRAC has been: how does it sense the swelling of a cell?
"People have scratched their heads over this for decades, because it's hard to imagine how a cell could directly measure an increase in its volume," Patapoutian said.
One possibility has been that VRAC senses a volume increase indirectly, by detecting the stretching of the cell membrane, as some sensory ion channels do. However, examining VRAC complexes in the simplified environment of lipid bilayers, the team found that they were not activated by membrane stretching. They were, however, readily activated when the usual concentration of dissolved ions was reduced.
That made sense. "Local decrease in the ionic strength is an inevitable result when the water rushes in and the cell swells," Syeda said.
Further studies of VRAC will be aimed at determining its precise physical structure, how variations in that structure alter its ion-conducting properties, how VRAC varies in different cell types, and how VRAC variants or mutants contribute to disease. VRAC is thought to worsen stroke-related brain damage and heart-attack damage, for example, by allowing abnormal, harmful flows of signaling molecules in the low-oxygen condition following arterial blockage. VRAC may also be linked to immune system development: a 2003 study found that a mutation of LRRC8A, now known to be VRAC's chief subunit, prevents antibody-producing B cells from developing normally. A more recent study implicated VRAC in the clinical response to the cancer drugs cisplatin and carboplatin—the drug molecules use VRACs as portals into tumor cells.
Journal information: Cell
Provided by The Scripps Research Institute