Insulin on demand: A biochemical explanation for the success of billion-dollar diabetes drugs
The protein targets of a class of 'blockbuster' diabetes drugs have been identified by A*STAR researchers and may help explain varying type-2 patient responses to the drugs.
Diabetes affects more than 400 million people worldwide—90 per cent of whom have developed type 2 diabetes—and the number is expected to surpass 600 million by 2040.
A study set out to determine why drugs that stimulate postprandial insulin secretion in people with type 2 diabetes have varying efficacy. "Understanding the mechanism of action of these drugs could help to explain why they are not as effective for particular subpopulations of diabetic patients," explains Weiping Han from the A*STAR Singapore Bioimaging Consortium, who led the study, in collaboration with researchers at Stanford University.
Normally after food intake, elevated blood glucose levels trigger an increase in calcium in pancreatic beta cells and signal the release of insulin. Insulin is an essential hormone for clearing the blood of excess glucose that cells use as energy.
In patients with type 2 diabetes, however, this glucose-to-insulin relay does not perform correctly. Drugs containing metabolic hormones, such as glucagon-like peptide-1 (GLP-1), have proven effective at boosting insulin secretion and restoring glucose homeostasis in these patients. Han and his colleagues sought the biological reason for the drugs' success.
Their previous study found that the membrane protein synaptotagmin-7 acts as a calcium sensor regulating insulin secretion in pancreatic beta cells.
In their most recent investigation, the researchers discovered that the same protein is a key target of the GLP-1 class of drugs. Specifically, they found that in the presence of glucose and calcium, GLP-1 triggers the phosphorylation of synapototagmin-7, which enhances insulin release. "This glucose dependence is ideal in preventing the risk of hypoglycemia," says Han. "When glucose levels return to normal, no matter how you modify the protein, you won't stimulate insulin secretion."
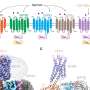
Han then used mass spectrometry chemical analysis to identify where on the protein phosphorylation occurs. Synaptotagmin-7 is made up of 403 amino acids with two large, distinct structural units responsible for binding to calcium. "We expected the phosphorylation to occur at one of these calcium binding sites, but it turned out to be at the linker region, serine-103," says Han. "This leaves room for the phosphorylation site to interact with other proteins." He is now trying to identify these interacting proteins.
The findings could also help explain other physiological functions where synaptotagmin proteins are at play, such as in the enhanced release of neurotransmitters from neurons during learning, memory and other higher-order brain activities, says Han.
More information: N. Gustavsson et al. Impaired insulin secretion and glucose intolerance in synaptotagmin-7 null mutant mice, Proceedings of the National Academy of Sciences (2008). DOI: 10.1073/pnas.0711700105
Bingbing Wu et al. Synaptotagmin-7 phosphorylation mediates GLP-1–dependent potentiation of insulin secretion from β-cells, Proceedings of the National Academy of Sciences (2015). DOI: 10.1073/pnas.1513004112
Journal information: Proceedings of the National Academy of Sciences