Stanford researchers urge lifting of NIH funding restrictions on chimeric research
Citing the "tremendous potential" of research on human stem cells in nonhuman embryos, scientists and a bioethicist from the Stanford University School of Medicine have co-authored a letter urging the removal of funding restrictions imposed on such research last month by the National Institutes of Health.
The researchers believe that work on what are called chimeric embryos is vital to advance our understanding of early human development, further our ability to accurately model devastating diseases and facilitate drug testing to ensure that potential therapies are safe and effective.
"Currently, it is impossible to accurately recapitulate human development in vitro, and there is no ethical method to obtain post-implantation stage human fetal tissue for isolating tissue and organ stem cells for regenerative medicine," they wrote.
The seven Stanford authors of the letter include Irving Weissman, MD, who directs Stanford's Institute for Stem Cell Biology and Regenerative Medicine, and David Magnus, PhD, director of Stanford's Center for Biomedical Ethics. The letter also was co-authored by four prominent scientists from other research institutions across the country.
It will be published in Science Nov. 6—the same day a workshop will be held at the NIH to discuss the restrictions and deliver new research guidelines.
"By eliminating federal funding for all aspects of this research, the NIH casts a shadow of negativity toward all experiments involving chimera studies regardless of whether human cells are involved," said assistant professor of medicine Sean Wu, PhD, MD, one of the senior authors of the letter. Weissman is the other co-senior author. "The current NIH restriction serves as a significant impediment to major scientific progress in the fields of stem cell and developmental biology and regenerative medicine and should be lifted as soon as possible."
Studying human cells in animals
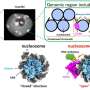
At issue is the growing field of research that seeks to understand how human pluripotent stem cells, which can become any cell type, may integrate and contribute to the development of a nonhuman animal, such as a laboratory mouse. Pluripotent stem cells can be isolated from human embryos or created in a lab from adult human cells, in which case they're known as induced pluripotent stem cells. Once obtained, these versatile cells can be injected into an early-stage animal embryo and studied as the embryo develops into an adult animal.
Tracking where these cells go and how they function in the growing embryo and the adult animal can help researchers understand early stages of human development that can't be studied any other way. (Although researchers can and do study the development of fertilized human eggs, the study period is restricted to only a few days after fertilization for ethical reasons.)
Furthermore, if cells from a person with a heritable disease, like sickle-cell disease, are used, it may be possible to generate an animal with the same disease for further experimentation or for testing to ensure drug safety before use in humans. Finally, if an animal is engineered to lack the ability to create a specific organ, such as a pancreas or liver, it may be possible for the human pluripotent stem cells to step up and develop an entirely human organ in that animal for study—or even for transplantation.
However, such studies have prompted ethical concerns, and in October the NIH abruptly suspended its funding of "research in which human pluripotent cells are introduced into nonhuman vertebrate animal pre-gastrulation stage embryos while the agency considers a possible policy revision in this area." The agency is hosting the Nov. 6 workshop of researchers and bioethicists from around the country to consider issuing new guidelines about the research.
Authors say concerns not supported by studies
The authors of the letter believe that concerns about the research are not supported by previous studies, and argue that an ongoing dialogue among scientists and bioethicists is sufficient to ensure the research is conducted in an ethically responsible manner.
"Much of the bioethical concern in regard to human/non-human chimerism arises from the possibility of chimeric animals harboring human neurons and germ cells. Can human neural cells co-exist with those from animals and establish 'humanized' cerebral anatomy and circuitries? Furthermore, would such chimeras be elevated to a higher metaphysical state and 'think' more like us? Current scientific data have not supported such possibilities, despite hundreds of xenotransplant studies introducing human neurons into the mouse brain," they wrote.
The researchers also cited current restrictions by the National Academy of Medicine and the National Research Council against breeding animals in which human pluripotent stem cells were implanted during development. These rules aim to prevent any possible transmission of human genes via the sperm or egg of the animal. They also pointed to the stricture against using nonhuman primates, which are considered too similar to humans, for such studies as reasonable boundaries for chimeric research.
"Ultimately, we believe that human/nonhuman chimerism studies in pregastrulation embryos hold tremendous potential to improve our understanding of early development, enhance disease modeling, and promote therapeutic discovery," they wrote.
More information: "Lift NIH restrictions on chimera research," by A. Sharma et al. Science, www.sciencemag.org/lookup/doi/ … ience.350.6261.640-a
Journal information: Science
Provided by Stanford University Medical Center