Graphene-coated heart valves could sidestep harmful drugs

Every year thousands of people are fitted with artificial heart valves to replace their own malfunctioning valve. Many of these patients, however, have to remain on drugs that stop blood clotting on these artificial valves. Now researchers have developed an artificial enzyme that would allow such patients to do away with such drugs altogether.
Medical implants that remain in contact with blood are common, from temporary catheters to artificial blood vessels. These devices cause the blood around them to clot, sometimes causing death. These clots can block blood vessels at the site of the device or elsewhere in the body, causing strokes and lethal embolisms.
Patients with permanent implants such as heart valves therefore have to take blood-thinning drugs, called anticoagulants, for the rest of their lives. These prevent blood clots from forming around the devices, reducing the risk of stroke and other complications. One of the most common anticoagulants given to these patients is warfarin, which requires careful and regular monitoring and is incompatible with many common drugs and some foods.
One alternative to avoid clotting is to use implants made from animal tissue rather than artificial materials. While this is an improvement, natural valves are prone to degradation and have to be surgically replaced.
Sugarcoated heart
Now researchers at the University of California at Los Angeles and the University of Michigan report in Nature Communications that they have come up with a third way which may allow long-lasting implants. They propose coating implants with a catalyst that uses the patient's own blood to make an anticoagulant called nitroxyl.
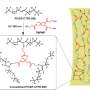
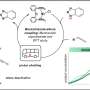
The coating catalyses – speeds up without participating in – two reactions in the blood near the implant. The catalysts are attached to a fragment of graphene – a single-atom layer of carbon – that holds the catalysts near each other. These catalysts convert glucose and an amino acid called L-arginine in the patient's blood to nitroxyl, which prevents clots from forming around the implant.
The first catalyst is a natural enzyme called glucose oxidase. This converts glucose in the blood to hydrogen peroxide, a common agent which is naturally present in the blood at low concentrations. The second catalyst is an artificial molecule called haemin which mimics another enzyme. Haemin promotes the reaction of hydrogen peroxide with L-arginine. Overall the molecule acts as an "artificial enzyme" for the cascade of reactions, mimicking the body's own anticoagulant production.
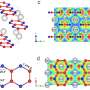
The graphene linker is a key development. Fragments of graphene consist of a flat sheet of carbon atoms dotted with imperfections. Haemin binds strongly to the flat regions of the molecule and adopts a shape that improves its function. The imperfections and the edges of the fragment contain functional groups which can be used to attach the glucose oxidase enzyme and allow the molecule to dissolve in water. Finally, graphene fragments of this kind are biocompatible: the body neither rejects nor damages the molecule.
Crucial questions remain before the new coating could be prepared for clinical use. If the coating is to be used on long-term implants, it must be shown to be stable and to remain active over decades. Its safety and side-effects must also be addressed: the haemin catalyst is not selective for L-arginine, and may well oxidise other molecules present in the blood and lead to unanticipated effects.
If the coating can be shown to be safe and stable, it may well offer relief to tens of thousands of people with blood-contacting implants who are would otherwise have to live on a diet of anticoagulants or face repeated surgery as tissue valves degrade.
Source: The Conversation
This story is published courtesy of The Conversation (under Creative Commons-Attribution/No derivatives).
![]()