Discovery of 'bioelectric' arteries opens path to heart disease treatment
Bionic eyes and limbs made television's six million dollar man an icon, but new research suggests our existing biological structure already exhibits a valuable electrical property. Scientists have found that arteries react curiously to external electric fields, opening the door to minimally invasive detection and treatment of the U.S.'s number one killer -- heart disease.
The research team found for the first time that electric charge inherently builds up along the walls of the body's largest artery, the aorta. The charge arranges itself so that an electric field points outward from the artery, and the direction of this internal field can be manipulated by external electric fields.
Together, these electrical traits make the aorta ferroelectric, a property mainly associated with artificial materials such as liquid crystals used in some flat screen displays. Although the researchers used pig tissue for their study, outside experts believe that these ferroelectric characteristics are likely present in humans as well.
"It's an unusual property, and we were very skeptical at the beginning," said Jiangyu Li, a mechanical engineer at the University of Washington, in Seattle, and a member of the research team. "It came to us as a big surprise, and we're very excited about it."
Having observed this property, scientists now hope to develop technology that takes advantage of it. Biomedical researchers envision new devices that could help abate the widespread problem of atherosclerosis, the buildup of fatty plaque in arteries.
Atherosclerosis occurs when excessive plaque in arterial walls blocks passageways and narrows blood's path to vital organs. Eventually, this bottlenecking can lead to heart attacks and strokes. Because electric charge builds up on plaque in a similar way to arteries, the interplay of these electrical properties might contribute to fat sticking to arterial walls.
Once the phenomenon is better understood, doctors could "apply the reverse process to help gradually reduce the plaque buildup," said Katherine Zhang, a biomedical engineer at Boston University and a coauthor of the research accepted for publication in the journal Physical Review Letters.
Required surgery would be minimally invasive, but researchers need to take several steps before this treatment option becomes a reality, said George Truskey, a biomedical engineer at Duke University who was unaffiliated with the research.
In addition to new treatments, this discovery may also lead to more accurate diagnostic techniques. Different types of plaque accumulate in arteries, and distinguishing between these types can guide doctors' prescribed treatments.
"One of the issues that cardiologists are trying to address is if a person has plaque, is it something they need to worry about?" said Truskey. "This method could help in determining the type of plaque."
Although proposed treatments and diagnostic tests remain speculative, basic research into bioelectricity has led to many medical applications in the past. Competing experiments by 18th century scientists Luigi Galvani and Alessandro Volta paved the way for research on bioelectricity and the eventual development of prosthetic limbs, ears and eyes.
But scientists are limited by what they can actually see. In the past, optical microscopes proved indispensable when scientists wanted to investigate the minute interactions of nerves and neurons. For this new research, the team had to look even closer.
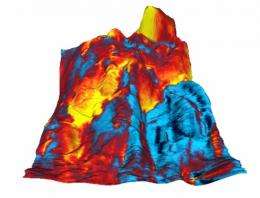
Li and his colleagues used a 20-nanometer-diameter conductive tip -- roughly the size of a virus -- to measure the electrical response of the tissue sample to an applied voltage. When the researchers applied a series of voltages, the charges rearranged themselves, effectively reversing the sample's electric field.
Being able to examine the arterial wall this closely may unravel some of the mystery behind arteries and help advance the growing field of tissue engineering. Current observation techniques limit the information that researchers can extract and simultaneously sacrifice the sample in the process.
"A big challenge is being able to non-destructively get information about the function and behavior of tissues," Truskey said. "If you can keep a tissue alive and monitor it, this gives you a much more powerful technique."
Research in this area is at a very early stage, and more work needs to be done to evaluate the benefits and risks of treatments that could use the aorta's ferroelectric properties, said Li. Nonetheless, Li and his colleagues hope that their discovery will generate interest in this research area and lead to anticipated treatments, diagnostic methods and advances in tissue engineering.
This research represents a first step in an emerging area of bioelectricity research, according to Truskey.
"Technically, it's a very impressive piece of work and a proof of principle," he said. "It opens up a lot of questions."
Journal information: Physical Review Letters
Source: Inside Science News Service