Decoding the proteins behind drug-resistant superbugs
Penicillin and its descendants once ruled supreme over bacteria. Then the bugs got stronger, and hospitals have reported bacterial infections so virulent that even powerful antibiotics held in reserve for these cases don't work.
To create the next line of defense against the most drug-resistant pathogens, scientists at the U.S. Department of Energy's Argonne National Laboratory and Texas A&M University have decoded the structure of a protein that confers drug resistance against our best antibiotics. The work could provide the foundation for new treatments to fight emerging drug-resistant superbugs.
β-lactam antibiotics are the most widely used antibacterials in the world because they effectively kill bacteria, but are minimally toxic to human cells—which means they have few side effects. But 1999 sounded the end of the reign of β-lactams. That year, a patient died in a Swedish hospital from an infection that didn't respond to antibiotics.
Penicillin was the original β-lactam, but as bugs evolved to fight it, scientists developed an entire family of related antibiotics, including amoxicillin, cephalexin and imipenem. The drugs work by blocking the bacteria's cell walls from growing normally. The latest class, called carbapenems, is generally held as the last line of defense against the toughest drug-resistant infections, like MRSA.
But bugs resistant even to carbapenems have begun spreading across the world, and they can trade this ability not only among each other but to other species of bacteria as well.
Scientists tracked down a gene that allows bacteria to resist these antibiotics, called NDM-1. The gene codes for a protein that latches onto part of the antibiotic molecule: the β-lactam ring that gives the family its name. The rings are rigid, and once they break apart, the antibiotic is useless. "That's why bacteria with NDM-1 genes are so deadly,” explained Andrzej Joachimiak, an Argonne Distinguished Fellow who co-authored the study.
But NDM-1's greatest trick is that it can disable the entire spectrum of β-lactam antibiotics. Each different antibiotic has a different molecular structure. Argonne researchers needed to know how one protein could break the rings in a dozen different configurations.
Joachimiak, who has a joint appointment with Argonne and the University of Chicago, took up the challenge with colleagues at the Midwest Center for Structural Genomics and Texas A&M University.
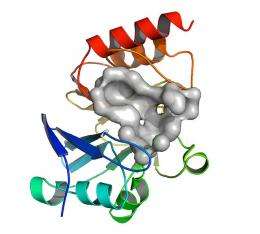
One of the most powerful tools in a biologist's kit is protein crystallography, which zooms down to the molecular level to get a picture of what the protein looks like. Protein crystals are tiny things: a thousand of them could sit side by side in a human hair. But intense X-rays from large synchrotrons like Argonne's Advanced Photon Source can be used as a "camera”: detectors collect the data from X-rays bouncing off the crystallized protein and use it to reconstruct the enzyme's structure, atom by atom.
The team managed to capture the NDM-1 enzyme in three different states. They found that NDM-1's active site, where it latches onto the antibiotic, is abnormally enormous, and flexible—like a mouth that is so large that it can capture the rings from a dozen different antibiotics, no matter their shape.
Decoding the structure allows scientists and companies to study the molecule for weaknesses: places where the structure could be attacked to disrupt its function. Joachimiak and the team are already beginning another study to test one way to neutralize the enzyme.
The study, "Structure of Apo- and Monometalated Forms of NDM-1—A Highly Potent Carbapenem-Hydrolyzing Metallo-β-Lactamase”, was funded by the National Institutes of Health and has been published online in the journal PLoS ONE/i>.
Provided by Argonne National Laboratory