Team reports major step forward in cell reprogramming

(PhysOrg.com) -- A team of Harvard Stem Cell Institute (HSCI) researchers has made a major advance toward producing induced pluripotent stem cells, or iPS cells, that are safe enough to use in treating diseases in patients.
“This demonstrates that we’re halfway home, and remarkably we got halfway home with just one chemical,” said Kevin Eggan, an HSCI principal faculty member who is the senior author of the paper being published online today by the journal Cell Stem Cell.
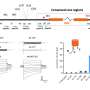
“There are four genes that do this, and with just one chemical we replaced half the genes,” said Eggan, who is also an assistant professor in Harvard’s Department of Stem Cell and Regenerative Biology. “The one chemical replaces those two genes in different ways at different times in the experiment. The experiments we performed not only led to discovery of the chemical, but they also explained how it works,” he said.
The chemical that the team used is a small molecule that members named RepSox in honor of another Boston team. It replaces Sox2 and cMyc, two of the four genes currently being used to reprogram adult skin cells into an embryonic-like state. Because cMyc is a tumor promoter and iPS cells created using it could never be used to treat patients, researchers have been looking for ways to turn back the cellular clock without the use of genes.
Lee Rubin, director of translational medicine at HSCI and the other senior author on the research team, said that “our goals were to try to as discretely and specifically as possible guide the cells through the deprogramming process” from the adult state to the embryonic-like state.
Finding a way to produce safe iPS cells that are the biological equivalent of embryonic stem cells is especially important because the cells can then be created from the cells of individual patients for transplantation into those patients. Thus, a patient with Parkinson’s disease might be treated with neurons created from his own cells, theoretically eliminating the need for immunosuppressive drugs, or the possibility of rejection of the transplanted cells. Similarly, patient-specific iPS cells could be used to create muscle for damaged hearts, or other individualized treatments.
Additionally, iPS cells derived from the skin cells of patients with specific diseases can be used as a source of differentiated cells to study those disease processes in a laboratory dish, and manipulated to find better drug targets and more effective therapeutics.
“This discovery is exciting because it demonstrates the feasibility of using chemicals to make safer patient-specific stem cells for transplantation medicine,” said Justin K. Ichida, a postdoctoral fellow in Eggan’s lab and the first author on the study. “One of the most important things we learned from this study is that, with respect to molecular pathways, there may be several ways to convert one type of cell into another. By using a nonbiased chemical screening approach, we uncovered a previously unknown way to make stem cells. The big challenge over the next decade will be to figure out how to make the right cells for disease treatment. This approach will be important for achieving that goal.”
Other co-first authors on the study are Joel Blanchard, Kelvin Lam, and Esther Y. Son. Additional contributors include Julia E. Chung, Dieter Egli, Kyle M. Loh, Ava C. Carter, Francesco P. Di Gorgio, Kathryn Koszak, Danwei Huangfu, Hidenori Akutsu, and David R. Liu.
More information: Cell Stem Cell: www.cell.com/cell-stem-cell/
Provided by Harvard University (news : web)