Bacteria 'launch a shield' to resist attack
Bacteria that cause chronic lung infections can communicate with each other to form a deadly shield against the body's natural defenses. Studying these interactions could lead to new ways of treating bacteria that are resistant to antibiotics, according to an article in the November issue of Microbiology.
Researchers from the University of Copenhagen and the Technical University of Denmark along with other collaborators in Denmark and the US found that the bacterium Pseudomonas aeruginosa can 'switch on' production of molecules that kill white blood cells - preventing the bacteria being eliminated by the body's immune system.
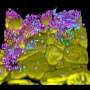
P. aeruginosa is responsible for many hospital-acquired infections and also causes chronic infections in those with pre-existing medical conditions such as cystic fibrosis (CF). The bacteria cause persistent lung infections by clumping together to form a biofilm, which spreads over the lungs like a slime. Such biofilms are generally resistant to antibiotics as well as the host immune response.
The study showed that P. aeruginosa uses a well-studied communication system called quorum sensing (QS) to detect approaching white blood cells and warn other bacteria in the biofilm. In response to this signal, the bacteria increase their production of molecules called rhamnolipids. These molecules sit on the biofilm surface to form a shield that destroys any white blood cells that encounter it. Interrupting quorum sensing to halt the "launch a shield" response could be a way of treating these bacteria that can resist antibiotics as well as the host immune system.
Professor Michael Givskov from the University of Copenhagen who led the study believes there are significant clinical benefits to this research. "The ultimate goal [of this research] is to eradicate the present day's antibiotic-resistant bacteria that are involved in the bulk of chronic infections," he says. "Antibiotic resistance is one of the most serious emerging health problems in the world today. More than 70% of the disease-causing bacteria are resistant to at least one of the currently available antibiotics. Studying interactions between P. aeruginosa and the innate and adaptive immune response will provide valuable information for the design of novel antimicrobials".
Source: Society for General Microbiology