Signal gradients in 3-D guide stem cell behavior
Scientists know that physical and biochemical signals can guide cells to make, for example, muscle, blood vessels or bone. But the exact recipes to produce the desired tissues have proved elusive.
Now, researchers at Case Western Reserve University have taken a step toward identifying that mix by developing an easy and versatile way of forming physical and biochemical gradients in three dimensions.
Ultimately, one of their goals is to engineer systems to manipulate stem cells to repair or replace damaged tissues and organs.
"If we can control the spatial presentation of signals, we may be able to have more control over cell behavior and enhance the rate and quality of tissue formation," said Eben Alsberg, an associate professor of biomedical engineering and orthopaedic surgery at Case Western Reserve and senior author of the research. "Many tissues form during development and healing processes at least in part due to gradients of signals: gradients of growth factors, gradients of physical triggers."
Alsberg, postdoctoral scholar Oju Jeon and graduate student Daniel S. Alt of Case Western Reserve, and Stephen W. Linderman, a visiting undergraduate on a National Science Foundation Research Experience for Undergraduates summer fellowship, tested their system on mesenchymal stem cells, turning them toward bone or cartilage cells. They report their findings in Advanced Materials.
Regulating the presentation of certain signals in three-dimensional space may be a key to engineering complex tissues, such as repairing osteochondral defects, damaged cartilage and bone in osteoarthritic joints, Alsberg said.
"There must be a transition from bone to cartilage," he said, "and that may require control over multiple signals to induce the stem cells to change into the different kinds of cells to form tissues where you need them."
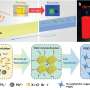
In their first test, the researchers found that stem cells changed into cartilage or bone cells in the directions of two opposing soluble growth factor gradients: one that promotes cartilage, called TGF-beta 1, and another that promotes bone, called BMP-2. The stem cells were placed in a solution of modified alginate, a material derived from seaweed that can form a jello-like material called a hydrogel when exposed to low level ultraviolet light.
The solution was divided between two computer-controlled syringe pumps, with BMP-2 in one syringe and TGF-beta 1 in the other. By controlling the rate of injection with the pumps and using a mixing unit, a hydrogel with a BMP-2 gradient starting with a large amount and tapering to nearly none and an opposing TGF-beta 1 gradient from low-to-high was formed.
The hydrogels were further modified in such a way that the growth factors were retained for a longer period of time. This enabled prolonged exposure of stem cells to the growth factors and further control over their differentiation into bone or cartilage cells.
The researchers then modified the hydrogel with a gradient of adhesion ligands, molecular strings that allow the stem cells to attach to the hydrogel itself. After two weeks of culturing the cells, they found the highest number of cells in the hydrogel region where the concentration of ligands was highest.
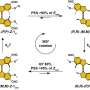
In a third test, they created a gradient of crosslink density within the hydrogels. Crosslinks provide structure to the gels. The lower the density, the more flexible the hydrogel; the higher, the stiffer the gel.
After two weeks, more cells were found in the most flexible gel regions within the gradient. The flexibility may allow for more free movement of nutrients and removal of waste products, Alsberg explained.
"This is exciting," Alsberg said. "We can look at this work as a proof of principle. Using this approach, you can use any growth factor or any adhesion ligand that influences cell behavior and study the role of gradient presentation. We can also examine multiple different parameters in one system to investigate the role of these gradients in combination on cell behavior."
If the technology enables them to unravel recipes that generate complex tissues, the biodegradable hydrogel mix could be implanted or injected at the site of an injury, the researchers say. The recipe would guide cell behavior until new tissue is formed, restoring function.
Journal information: Advanced Materials
Provided by Case Western Reserve University