One nanoparticle plus one antibody equals targeted drug delivery to tumors
(Phys.org) —Herceptin and camptothecin are both powerful anticancer agents with key characteristics that limit their effectiveness in treating cancer. Patients treated with Herceptin, a monoclonal antibody that targets a growth promoting factor common to breast cancers (Her2), often relapse as their tumors become resistant to the drug. overcoming camptothecin"s toxicity and low solubility represent major therapeutic challenges. Now, researchers at the California Institute of Technology have used nanotechnology to combine the two into what so far appears to be a highly effective drug for treating aggressive breast cancer.
Mark E. Davis and his graduate student Han Han report their developmental work in the journal Molecular Pharmaceutics. Dr. Davis is also a project leader at Caltech's Center of Cancer Nanotechnology Excellence.
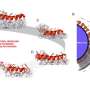
Drugs based on monoclonal antibodies and nanoparticles are not new, but what Dr. Davis and Ms. Han have done for the first time is use a single antibody molecule, bound to a nanoparticle, as both a targeting agent for that drug-loaded nanoparticle and a therapeutic agent. They created this construct by first linking insoluble camptothecin to a natural biopolymer known as mucin and the widely used biocompatible polymer, polyethylene glycol (PEG). The camptothecin-mucin-PEG combination self-assembles into a tightly packed nanoparticle that readily dissolves in water and biological fluids such as blood. They then chemically linked one molecule of Herceptin per nanoparticle to create their final therapeutic agent.
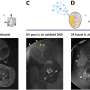
In a previous study the group showed that a line of aggressive breast tumor cells that overexpress the Her2 protein readily took up the Herceptin-linked nanoparticle. Based on these results, the Caltech researchers conducted tests in mice with tumors grown from this same cell line, which cancer researchers consider one of the most resistant cell lines to anticancer drugs, including camptothecin. First, they determined the maximum tolerated dose of the camptothecin nanoparticle drug without Herceptin, that is, the highest dose that would not cause the mice to lose more than 15 percent of their body weight. They then treated tumor-bearing animals with a dose of the Herceptin-bound nanoparticle that was approximately 10 percent of this maximum tolerated dose.
The results were impressive. All animals that received the Herceptin-camptothecin nanoparticle were free of any evidence of tumor by day nine of the experiment after a single injection, and the animals remained tumor-free at the end of the six week study (while being injected every three weeks). Animals treated with an equivalent amount of Herceptin alone every two weeks or untargeted camptothecin-loaded nanoparticles responded positively, with the majority of the treated mice showing significant tumor shrinkage, though only half the animals experienced complete tumor regression. Tumors grew rapidly with no signs of positive response in animals that received either saline or free camptothecin and none of the animals in those two groups survived to the end of the study.
This research, which is detailed in a paper titled, "Single-antibody, targeted nanoparticle delivery of camptothecin," was supported by the NCI Alliance for Nanotechnology in Cancer, a comprehensive initiative designed to accelerate the application of nanotechnology to the prevention, diagnosis, and treatment of cancer. An abstract of this paper is available at the journal's website.
Journal information: Molecular Pharmaceutics
Provided by National Cancer Institute