Tear drops may rival blood drops in testing blood sugar in diabetes
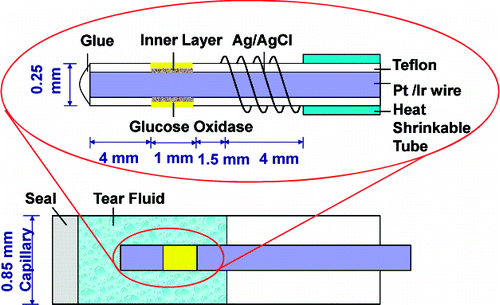
Scientists are reporting development and successful laboratory testing of an electrochemical sensor device that has the potential to measure blood sugar levels from tears instead of blood — an advance that could save the world's 350 million diabetes patients the discomfort of pricking their fingers for droplets of blood used in traditional blood sugar tests. Their report appears in ACS' journal Analytical Chemistry.
Mark Meyerhoff and colleagues explain that about 5 percent of the world's population (and about 26 million people in the U.S. alone) have diabetes. The disease is a fast-growing public health problem because of a sharp global increase in obesity, which makes people susceptible to developing type 2 diabetes. People with diabetes must monitor their blood glucose levels several times a day to make sure they are within a safe range. Current handheld glucose meters require a drop of blood, which patients draw by pricking their fingers with a small pin or lancet. However, some patients regard that pinprick as painful enough to discourage regular testing. That's why Meyerhoff's team is working to develop a new, pain-free device that can use tear glucose levels as an accurate reflection of blood sugar levels.
Tests of their approach in laboratory rabbits, used as surrogates for humans in such experiments, showed that levels of glucose in tears track the amounts of glucose in the blood. "Thus, it may be possible to measure tear glucose levels multiple times per day to monitor blood glucose changes without the potential pain from the repeated invasive blood drawing method," say the researchers.
More information: Measurement of Tear Glucose Levels with Amperometric Glucose Biosensor/Capillary Tube Configuration, Anal. Chem., 2011, 83 (21), pp 8341–8346. DOI: 10.1021/ac201700c
Abstract
An amperometric needle-type electrochemical glucose sensor intended for tear glucose measurements is described and employed in conjunction with a 0.84 mm i.d. capillary tube to collect microliter volumes of tear fluid. The sensor is based on immobilizing glucose oxidase on a 0.25 mm o.d. platinum/iridium (Pt/Ir) wire and anodically detecting the liberated hydrogen peroxide from the enzymatic reaction. Inner layers of Nafion and an electropolymerized film of 1,3-diaminobenzene/resorcinol greatly enhance the selectivity for glucose over potential interferences in tear fluid, including ascorbic acid and uric acid. Further, the new sensor is optimized to achieve very low detection limits of 1.5 ± 0.4 μM of glucose (S/N = 3) that is required to monitor glucose levels in tear fluid with a glucose sensitivity of 0.032 ± 0.02 nA/μM (n = 6). Only 4–5 μL of tear fluid in the capillary tube is required when the needle sensor is inserted into the capillary. The glucose sensor was employed to measure tear glucose levels in anesthetized rabbits over an 8 h period while also measuring the blood glucose values. A strong correlation between tear and blood glucose levels was found, suggesting that measurement of tear glucose is a potential noninvasive substitute for blood glucose measurements, and the new sensor configuration could aid in conducting further research in this direction.
Provided by American Chemical Society