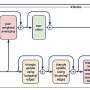
Stem cell hierarchy offers potential for isolating, growing cells
Researchers at the University of Toronto Institute of Biomaterials and Biomedical Engineering (IBBME) and Princess Margaret Hospital (PMH), led by U of T's Professor J.E. Davies, have made important progress in stem cell research that will allow for numerous applications of multi-faceted stem cells known as mesenchymal stem cells (MSCs). This research will advance the selection of specific cells to target specific diseases, ultimately enabling clinicians to "personalize" treatment for patients.
The important research published today in the Public Library of Science journal, PloS-ONE [www.plosone.org/home.action], is entitled Human Mesenchymal Stem Cells Self-Renew and Differentiate According to a Deterministic Hierarchy. The paper represents the work of Davies' fellow investigators Professors William Stanford (IBBME) and Armand Keating (director, cell therapy program, PMH) and their jointly supervised students Rahul Sarugaser and Lorraine Hanoun.
The paper finally provides the experimental proof of the existence of a human MSC at the single cell level, a key step that has previously eluded the scientific community. The researchers have for the first time, defined a mesenchymal stem cell hierarchy that introduces the possibility of isolating and growing MSCs of different capacities for different clinical applications or drug discovery.This development builds on the team's previous finding that the richest source of MSCs in the body is found in umbilical cord tissue that is normally discarded at birth.
"The significance of this discovery is huge," Davies said. "These cells are quite different to blood stem cells; they are thought to give rise to all the so-called connective tissues of the body including bone, cartilage, muscle, tendons and ligaments. Also, unlike blood stem cells, MSCs are considered to be immune-privileged, meaning that donor and recipient don't need to be matched."
Pre-clinical work is already showing promising results for the practical applications for these stem cells. Davies and his team report implanting MSC cells derived from what is effectively medical waste, into bone marrow cavities and observing that the cells both stimulate and contribute to the formation of new bone and cartilage. In separate experiments they have also shown that the cells can accelerate skin wound healing, and also have all the immune-regulatory properties known to be important in the treatment of many diseases.
Beyond its promise for healing, Dr. Davies says the discovery has other important implications for research and health care.The team is working with adult stem cells which are not subject to either the ethical or scientific concerns associated with the use of embryonic stem cells. And this pioneering work can provide cost savings because today, the close to 60 MSC trials in progress throughout the world depend upon volunteers providing some of their bone marrow to harvest a much smaller population of MSCs. With 130 million babies born every year, the umbilical cord represents a virtually inexhaustible and accessible source of cells.
"From a clinical perspective," said Keating, "characterization of these MSCs at a single cell level may provide an opportunity to identify stem cells that may be particularly effective in regenerating specific tissues and organs. As a next step, once the pre-clinical studies have been completed, we can take advantage of the existing state-of-the-art good panufacturing practice-level facilities at Princess Margaret Hospital and University Health Network to manufacture clinical-grade cells for clinical use."
Davies founded Tissue Regeneration Therapeutics Inc. (TRT) in 2004, and obtained a United States patent earlier this year for his first discovery. The cell harvesting technology was licensed, by TRT, to CReATe Cord Blood Bank in Toronto and now a growing number of Canadian parents are using CReATe's services to store these very special MSCs (marketed as Peristem™) at the birth of their children - along with the umbilical cord blood which is stored as a source of blood stem cells.
Provided by University of Toronto (news : web)