Identification of genes that cause resistance to treatment of the pathogenic fungus Candida
It is estimated that 80% of women will suffer from vaginal candidiasis at least once in their lives. In addition to superficial infections, which can be oral or vaginal and do not usually have a serious prognosis, fungi of the Candida genus can cause systemic diseases in immunocompromised individuals and these are fatal in 40% of cases. Drugs are available to treat these conditions, but doctors are increasingly encountering varieties of fungi that have developed resistance to treatments, thus making candida infection a serious global health problem.
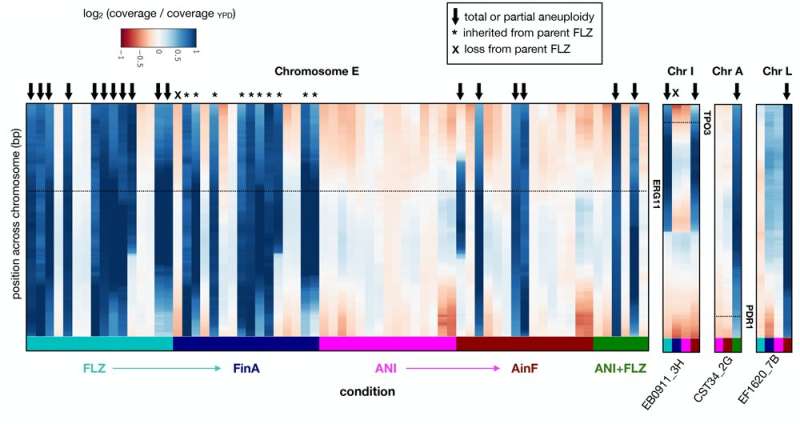
Scientists led by Dr. Toni Gabaldón, ICREA researcher and group leader at the Institute for Research in Biomedicine (IRB Barcelona) and the Barcelona Supercomputing Center (BSC), have studied the resistance mechanisms developed by the species Candida glabrata upon exposure to various drugs and have identified eight genes that, when mutated, are responsible for allowing the fungus to adapt and survive treatment. To date, only half of these genes were known as candidates to confer drug resistance.
"The interesting thing about this work is that the identification of these eight genes allows us to use a genetic test to diagnose potential drug resistance present in the infection of a specific patient and, therefore, help choose the best treatment," says Dr. Gabaldón, head of the Comparative Genomics lab at IRB Barcelona.
Evolutionary process underlying the incorporation of resistance mechanisms
To perform this study, the researchers cultured independent populations of the fungus Candida glabrata and administered a variety of drugs available on the market that have different mechanisms of action. They then analyzed the resistance developed and the genomes of the distinct populations to correlate the mechanisms with the genetic differences.
The strains that have been generated in this work, which combine resistance to several drugs, can serve as a study model in the search for new treatments.
Cross-resistance phenomena
In addition to resistance to the treatment administered, the researchers observed that exposure to one particular drug (fluconazol) also caused resistance to another type of drug (equinocandina) in 50% of the cases, although these populations had never been exposed to the second drug.
"This phenomenon is known as cross-resistance and, in this regard, our discoveries should lead to an adaptation of treatment guidelines to avoid favoring the appearance of multiresistance," says Dr. Gabaldón.
The research was published in Current Biology.
More information: Ewa Ksiezopolska et al, Narrow mutational signatures drive acquisition of multidrug resistance in the fungal pathogen Candida glabrata, Current Biology (2021). doi.org/10.1016/j.cub.2021.09.084
Journal information: Current Biology