Study shows how meningitis-causing bacteria may sense fever to avoid immune killing
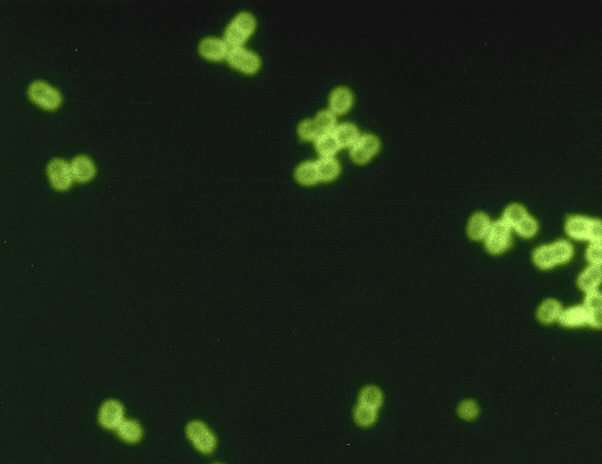
Researchers at Karolinska Institutet in Sweden have discovered a mechanism through which meningitis-causing bacteria can evade the immune system. In laboratory tests, they found that Streptococcus pneumoniae and Haemophilus influenzae respond to increasing temperatures by producing safeguards that keep them from getting killed. This may prime their defenses against our immune system and increase their chances of survival, the researchers say. The findings are published in the journal PLoS Pathogens.
"This discovery helps to increase our understanding of the mechanisms these bacteria use to evade our normal immune defenses," says co-corresponding author Edmund Loh, researcher in the Department of Microbiology, Tumor and Cell Biology at Karolinska Institutet. "It could be an important piece of the puzzle in examining what turns this usually harmless bacterium into a lethal killer."
Meningitis is an inflammation of the membranes surrounding the brain and the spinal cord. It can be caused by viruses, bacteria, fungi and parasites.
Bacterial meningitis is one of the most severe types and a major cause of death and disability in children worldwide. Several kinds of bacteria can cause the infection, including the respiratory pathogens Streptococcus pneumoniae and Haemophilus influenzae, which can be attributed to some 200,000 meningitis-caused deaths annually.
These two bacteria often reside in the nose and throat of healthy people without making them ill. In some cases they spread into the bloodstream and cause invasive diseases, but the reasons for this remain largely unknown.
In this study, the researchers set out to investigate the connection between temperature changes and survival of these bacteria in a laboratory setting. The experiments were prompted by another recent finding that linked the temperature sensing abilities of the bacterium N. meningitidis to invasive meningococcal disease.
One of the signs of an infection is elevated temperatures and fever, which typically boost our immune system's ability to fight illness. In this study, however, the researchers found that both S. pneumoniae and H. influenzae activated stronger immune protections when challenged with higher temperatures.
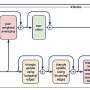
They did so through mechanisms involving four specific so-called RNA thermosensors (RNATs), which are temperature-sensitive non-coding RNA molecules. These RNATs helped boost the production of bigger protective capsules and immune modulatory Factor H binding proteins, both of which help shield these bacteria from immune system attacks.
"Our results indicate that these temperature sensing RNATs create an additional layer of protection that helps the bacteria colonize their normal habitat in the nose and throat," says the paper's first author Hannes Eichner, Ph.D. student at the same department. "Interestingly, we saw that these RNATs do not possess any sequence similarity, but all retain the same thermosensing ability, which indicates that these RNATs have evolved independently to sense the same temperature cue in the nasopharynx to avoid immune killing."
More research is needed to understand exactly what triggers these pathogens to breach from the mucous membrane into the bloodstream and further into the brain. Future studies encompassing in vivo infection model are warranted to characterize the role of these RNATs during colonization and invasion, the researchers say.
More information: "RNA thermosensors facilitate Streptococcus pneumoniae and Haemophilus influenzae immune evasion," Hannes Eichner, Jens Karlsson, Laura Spelmink, Anuj Pathak, Lok-To Sham, Birgitta Henriques-Normark, Edmund Loh, PLoS Pathogens, online April 29, 2021, DOI: 10.1371/journal.ppat.1009513
Journal information: PLoS Pathogens
Provided by Karolinska Institutet