Engineered 'nanobodies' block SARS-CoV-2 from infecting human cells
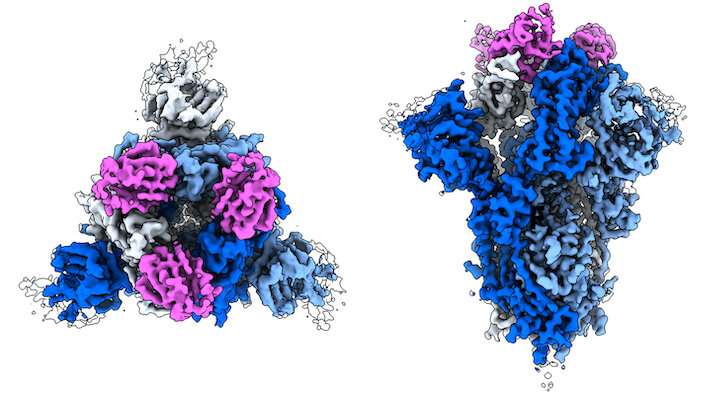
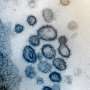
Researchers have designed a molecule that sticks tightly to the coronavirus spike protein, preventing the virus from infecting cells. The molecule might someday be used in an aerosolized drug to treat or prevent COVID-19.
In the race to find drugs that halt the novel coronavirus, scientists are finding inspiration in unusual sources—like llamas.
A new lab-engineered molecule inactivates the machinery that the coronavirus, SARS-CoV-2, uses to infect cells. It's modeled after the simple, compact antibodies found in some animals such as llamas, alpacas, and camels.
While the research is still preliminary, the team behind the advance hopes their molecule might someday be the key ingredient in an antiviral drug that could be delivered via nasal spray.
"In just twelve weeks, we've found a molecule that's a clinical lead," says Howard Hughes Medical Institute Investigator Peter Walter, a biochemist at the University of California, San Francisco (UCSF), who co-led the work. The team described the advance August 17, 2020, in a preprint posted to bioRxiv.org.
Alongside vaccines, drugs that target SARS-CoV-2 are important tools for keeping the COVID-19 pandemic in check. Researchers have identified existing drugs that can be repurposed to treat symptoms of the virus and help quell severe infections. But a drug specifically designed to attack SARS-CoV-2 might be more effective at halting the virus in its tracks before it causes severe disease, Walter says. To make such drugs, he and others are designing custom antibodies.
Immune cells produce antibodies in response to infection, but it takes time for that response to develop. Lab-made antibodies could knock a virus out before it gains a foothold.
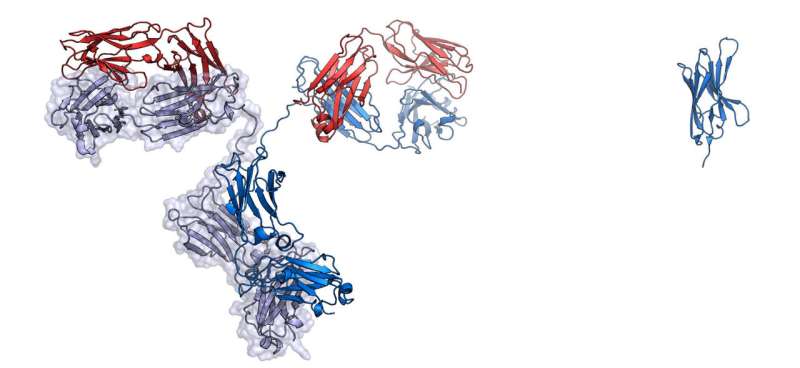
That's where the llamas come in. Alpacas and llamas have a simpler version of the antibodies found in humans—only a tenth the size, with fewer components. These stripped-down antibodies, called "nanobodies," are potentially powerful drug building blocks, says Aashish Manglik, a protein engineer at UCSF who co-led the study with Walter. "Because of their unique shape they can often fit deep inside the crevices of proteins." They tend to be more stable than regular antibodies, too.
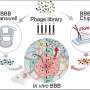
Manglik's lab has developed large collections of these synthetic proteins as a resource for drug discovery. When the COVID-19 pandemic began, these collections were the perfect place to hunt for a molecule that could deactivate SARS-CoV-2, Walter says.
Michael Schoof, a graduate student in Walter's lab, began mining Manglik's nanobody collections en masse. The aim: Finding any nanobodies that would stick to the coronavirus spike protein, the key on the virus's surface that lets it sneak into cells.
In a series of lab experiments, he and his colleagues winnowed down a pool of billions of different nanobodies to a few dozen that stuck strongly to the spike protein. Then, they engineered the most promising candidate, linking three copies of the same nanobody together into a chain.
That three-piece molecule wedged tightly against the virus spike protein, pinning it into a shape that prevented attachment to human cells. The researchers also discovered that the molecule is particularly sturdy. In test-tube experiments, a single nanobody fell off the spike protein within minutes. The team calculated that the three-piece version would be able to hold on for over a week without budging.
The work hasn't yet been peer-reviewed, but Walter and Manglik are currently looking for partners who can produce and test the molecule for safety and efficacy in clinical trials. They hope the molecule could someday soon work as an aerosolized drug that would get directly to patients' lungs.
Traditional antibody drugs are usually injected into the patient's bloodstream—most antibodies fall apart when aerosolized by a nebulizer or a nasal spray, Walter says. Preliminary tests suggest that the new nanobody-based molecule is far hardier. The nanobodies kept their shape and function when sprayed, and withstood being freeze-dried and heated, too.
Aerosolized delivery of a nanobody drug "is an exciting possibility, but it hasn't been demonstrated yet," says Andrew Kruse, a biochemist at Harvard Medical School who has collaborated with Manglik's team to build nanobody collections but wasn't involved in the current study. "It would be very important to see how long an aerosol-delivered nanobody remains in the respiratory system," he says.
More information: Michael Schoof et al. An ultra-potent synthetic nanobody neutralizes SARS-CoV-2 by locking Spike into an inactive conformation, (2020). DOI: 10.1101/2020.08.08.238469
Provided by Howard Hughes Medical Institute